Site Search
743 results for access here PROBLEMGO.com Need a bondsman who takes payment plans for release today
-
5 Things You Need to Know About Equitable Generations Universal Life
Here are five things you need to know about Equitable Generations™ Universal Life
1. Affordability
Because Equitable Life is owned by its policyholders, we don’t have to worry about paying shareholders. That means we can focus on offering competitive pricing!
2. Investments
Equitable Generations Universal Life is built for the 21st century with investment options that matter to today’s buyer including Target date, Environmental, Social, and Governance (ESG) funds for sustainable investing.
3. Fees
Equitable Generations has eliminated most universal life fund administration fees as well as the policy administration fee.
4. KIND™
Equitable Generations has a suite of contractual and non-contractual claims features we call KIND, designed to help your family navigate the claims process with ease.
5. FlexibilityWith such competitive pricing, fantastic investment options and minimal fees. Equitable Generations Universal Life provides a level of flexibility rarely seen in the Universal Life space.
See Equitable Generations Universal Life for yourself within one minute - try the EZStart quick quote software for advisors, available on EquiNet!
Please contact your local wholesaler for more information.
TM and ® denote trademarks of The Equitable Life Insurance Company of Canada. - What's new?
-
Individual insurance communications at Equitable are changing
Out with the old and in with the new … in phases. Less than one year after the launch of our bold brand redesign, we are refreshing Equitable® individual insurance client letter communications. The updated letters are an opportunity to show more than our new logo. It’s about showing clients that we are here to listen and support them every step of the way.
This fresh approach to client communication delivers greater personalization that evolves with each client’s needs. Adopting a more inclusive and conversational tone means clients will stay well informed with clarity, so they can understand their insurance policies and the claims process better. Consistent communication across their insurance journey with Equitable reinforces how much we value their trust in us to support their financial needs.
Other notable changes you can expect to see over the next year include:
● Graphic icons
● Scannable content
● Simplified layouts
● Visual financial data
The rollout of new letters begins this fall. As always, you can access a copy of your clients’ letters on EquiNet®.
Questions or want to share feedback? Talk to your Equitable wholesaler today!
® or TM denote trademarks of The Equitable Life Insurance Company of Canada. - Life Policy Collateral Loans
-
Tax impacts of the Canadian Dental Care Plan for your clients
Tax impacts of the Canadian Dental Care Plan for your clients*
Earlier this year, the government shared its progress on the Canadian Dental Care Plan (CDCP).
The CDCP will be available to Canadians with an annual family income of less than $90,000 who do not have dental benefits. Co-pays will be waived for eligible Canadians with a family income of less than $70,000.
Canadians who have access to private dental coverage are not eligible for the CDCP. This means that your clients must now report on T4s/T4As if dental coverage** was available on December 31 of the reporting tax year for:- Employees,
- Employees’ spouses and/or dependents,
- Former employees, and
- Spouses of deceased employees.
This new tax reporting requirement is mandatory starting with the 2023 tax year. Employee tax slips will include new boxes for employers to complete:- Box 45 (T4): Employer Offered Dental Benefits. This new box will be mandatory.
- Box 015 (T4A): Payer Offered Dental Benefits. This new box will be mandatory if plan sponsors report in Box 016, Pension or Superannuation. The box will otherwise be optional.
- Code 1: The plan member has no access to dental care insurance or coverage of dental services of any kind.
- Code 2: Only the plan member has access to any dental care insurance, or coverage of dental services of any kind.
- Code 3: The plan member, their spouse and their dependents have access to any dental care insurance, or coverage of dental services of any kind.
- Code 4: Only the plan member and their spouse have access to any dental care insurance, or coverage of dental services of any kind.
- Code 5: Only the plan member and their dependents have access to any dental care insurance, or coverage of dental services of any kind.
Reports for dependents
We have a report available for plan members who have enrolled their dependents in benefits coverage. Your clients can contact their local service team representative to receive a copy of the report. We are working to make it available on our Advisor and PA websites.
Questions
For guidance on your tax slips and reporting obligations, please encourage your clients to contact their accountant, payroll provider or tax advisor.
Supporting plan members affected by the Israeli-Palestinian conflict*
Traumatic events continue to unfold in the Middle East. Enduring ongoing news of conflict and suffering could challenge many Canadians. During this difficult time, Equitable encourages affected clients and plan members to access the mental health support they need.
Large-scale traumatic news events can cause people to experience intense reactions. This puts a lot of strain on their mental health. Having coping mechanisms to deal with the current crisis can be a huge help. Any Equitable Life plan member who needs mental health support can visit Homeweb.ca/equitable to access online resources or contact Homewood at 1.888.707.2115.
Support available to all Equitable plan members
Support available to plan members with the Homewood Health EFAP
For your clients that have purchased Homewood Health’s Employee and Family Assistance Program (EFAP), remind them that their plan members also have access to confidential counselling services. The EFAP provides plan members with 24/7 access to confidential counselling through a national network of mental health professionals. Whether it’s face-to-face, by phone, email, chat or video, plan members and their dependent family members will receive appropriate, timely support for the issue they’re dealing with.
Questions?
If you need more information, contact your Group Account Executive or myFlex account executive.
*Indicates content that will be shared with your clients. -
Most employers staying the course on benefits during COVID-19
With businesses suffering hardship due to COVID-19, employers are turning to you for advice on their benefits plans during these difficult times. We’ve received numerous questions from advisors about changes our clients are making to their plans during this crisis.
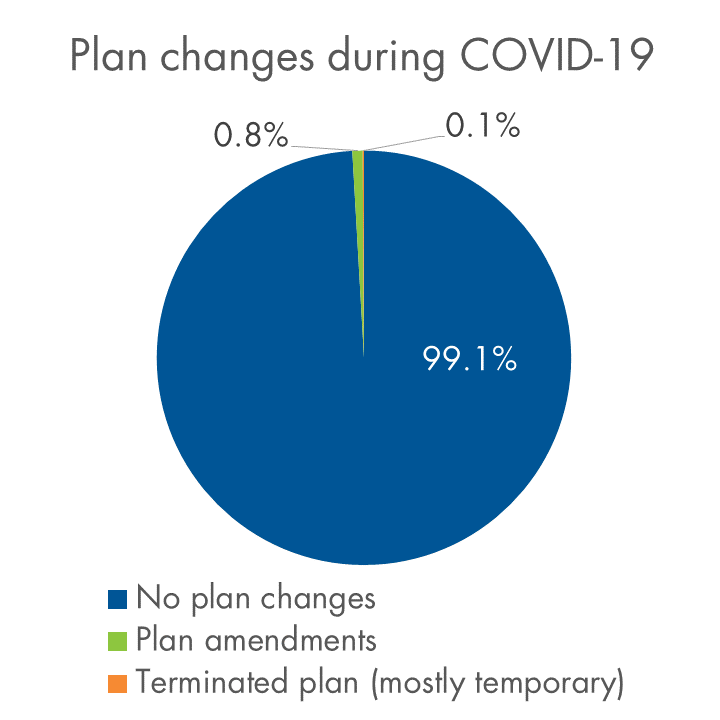
So far, the vast majority of clients are standing pat and taking a wait-and-see approach. Plan amendments have been the exception – fewer than 1% of our clients have made COVID-19-related amendments as of mid-April. Almost all are clients with fewer than 50 lives.
We know that many of our clients have experienced layoffs, but hardly any have cancelled benefits. Fewer than 0.1% have terminated benefits to date.
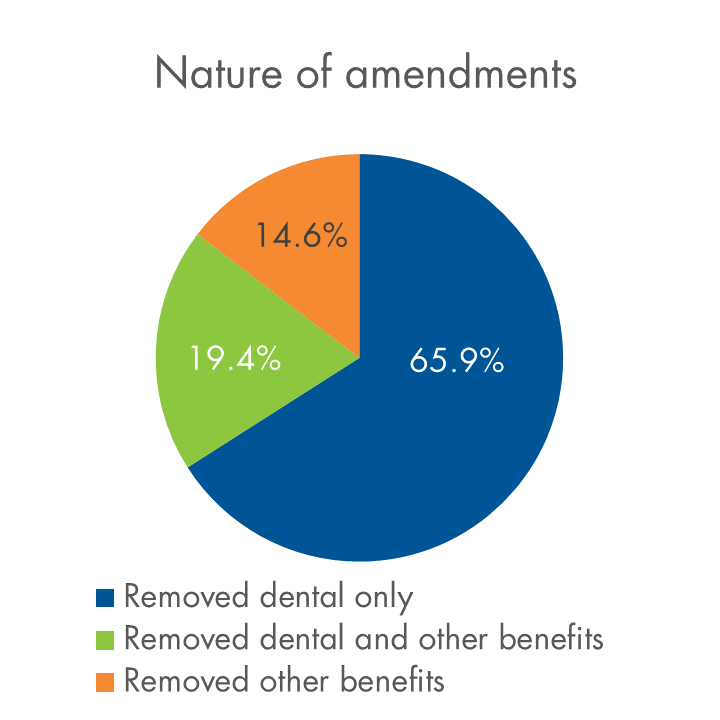
Below is a snapshot of plan amendments and terminations relative to our overall block, and an overview of the types of amendments we’re seeing.
COVID-19-related plan changes on Equitable Life’s block of businessAs of April 15, 2020
Have clients who need to make a change?
We know this is a difficult time for Canadian employers. If you have a client who needs to make a change to their plan, please contact your Group Account Executive or myFlex Sales Manager. We have a range of options to help them manage, and changes can be made quickly. The average turnaround time for COVID-19-related amendments is currently about four days.
We’re happy to work with each employer to understand the options that suit their specific situation best.
- [pdf] Equitable GIF TFSA Application
-
February 2023 eNews
Responding to Nova Scotia’s biosimilar switch initiative
We are changing coverage for some biologic drugs in Nova Scotia in response to the province’s biosimilar initiative. These changes will help protect your clients’ plans from additional drug costs that may result from this new government policy while providing access to equally safe and effective lower-cost biosimilars.Nova Scotia’s provincial biosimilar initiative
Announced in February 2022, the Nova Scotia Biosimilar Initiative ends coverage of seven biologic drugs for residents enrolled in Pharmacare programs.
Pharmacare patients in the province using these drugs will be required to switch to biosimilar versions of these drugs by February 3, 2023, in order to maintain their Nova Scotia Pharmacare coverage.Equitable Life’s response
To ensure this provincial change doesn’t result in your clients’ plans paying additional and avoidable drug costs, we are changing coverage in Nova Scotia for most biologic drugs included in the provincial initiative.
Beginning June 1, 2023, plan members in the province will no longer be eligible for most originator biologic drugs if they have a condition for which Health Canada has approved a lower cost biosimilar version of the drug.** These plan members will be required to switch to a biosimilar version of the drug to maintain coverage under their Equitable Life plan.Can my client maintain coverage of these biologic drugs?
Traditional groups who wish to opt out of this change and maintain coverage of these originator biologics for Nova Scotia plan members can submit a policy amendment. Amendments must be submitted no later than April 1, 2023. Advisors with myFlex Benefits clients who wish to maintain coverage of these originator biologics for Nova Scotia plan members should speak to their myFlex Sales Manager to confirm their eligibility to opt out of this change.
Groups that choose to maintain coverage of these originator biologics for existing claimants will also maintain coverage for any originator biologics that we subsequently add to our Nova Scotia biosimilar initiative.Will this change impact my clients’ rates?
The rate impact of this change in coverage will be relatively insignificant. Any cost savings associated with the change will be factored in at renewal.
If plan sponsors opt out of these changes and maintain coverage for the originator biologics, it may result in a rate increase. Any rate adjustment will be applied at renewal.Communicating this change to plan members
We will inform any affected plan members in April of the need to switch their medications so that they have ample time to change their prescriptions and avoid any interruptions in treatment or coverage.What is the difference between biologics and biosimilars?
Biologics are drugs that are engineered using living organisms like yeast and bacteria. The first version of a biologic developed is known as the “originator” biologic. Biosimilars are highly similar to the drugs they are based on and Health Canada considers them to be equally safe and effective for approved conditions.Questions?
If you have any questions about this change, please contact your Group Account Executive or myFlex Sales Manager.
**The list of affected drugs is dynamic and will change as Nova Scotia includes more biologic drugs in its biosimilar initiative, as new biosimilars come onto the market, and as we make changes in drug eligibility.
Changes to New Brunswick drug interchangeability rules
We are introducing changes to help ensure that your clients with voluntary or mandatory generic pricing for their drug plans will benefit more from the cost savings of these two features, regardless of the province where the drugs are dispensed.
Currently, when determining whether a lower-cost alternative is available for a brand-name drug, most insurers only consider drugs that the provincial drug plan identifies as interchangeable.
However, the public drug plan in New Brunswick does not identify a drug as interchangeable if the drug is not listed on its formulary – even if Health Canada has deemed the drug interchangeable.
As a result, plans with mandatory or voluntary generic pricing have continued to reimburse some drugs in New Brunswick based on the cost of the brand-name drug, even if a lower-cost generic alternative is available.
Effective March 20, 2023, if your clients have drug plans with mandatory or voluntary generic pricing, we will adjudicate any drug claims in New Brunswick using the lowest cost alternative that Health Canada approves as bioequivalent. This will occur even if the public drug plan has not identified the drug as interchangeable.
To benefit from this more robust drug plan control, plan sponsors must have mandatory or voluntary generic pricing in place.
For more information about this change or about implementing mandatory or voluntary generic pricing for your clients, please contact your Group Account Executive or myFlex Sales Manager.
New template: plan members eligible for additional coverage
Often, based on salary, some plan members may become eligible to apply for extra Life, Accidental Death & Dismemberment (AD&D), Short Term Disability or Long Term Disability coverage. If this occurs, your clients receive a notification from Group Benefits Administration. We have now developed a template that your clients can provide to applicable plan members if they become eligible for extra coverage. The template makes it simpler for your clients to pass on these details to their plan members efficiently.
The new template is available for download under the Quick Links section of EquitableHealth.ca. It is a fillable PDF form that your clients can complete and provide to their plan members when necessary. The document is called Over the Non-Evidence Limit for Plan Members Notification.
If you have any questions about the template, please contact your Group Account Executive or myFlex Sales Manager. - Benefits and Key features
- [pdf] Borrowing money to save money
