Site Search
770 results for PROBLEMGO.com Paying to have an arrest record sealed dark web browse here anonymity guaranteed now
- Step Up Your Wealth Sales program
-
Get the Straight Talk on Equitable’s par account performance
Real answers to big questions
At Equitable, we understand how important it is to make confident decisions when dealing with large cases. When you have questions, you need concise, direct insights from leaders and subject matter experts.
Introducing the Straight Talk video series
Today, we are thrilled to share the first episode of Straight Talk. This episode features Mark Arruda, VP of Individual Insurance Pricing and Finance.
Mark talks about how Equitable’s par account is built to perform in all kinds of conditions, with strong governance, disciplined risk management, and prudent capital practices that ensure stability even when large life insurance claims are paid out.
Watch Straight Talk for straight answers to the questions that matter most.
Contact your Equitable Wholesaler to learn more about Equimax.
-
Insights from a pandemic: Drug trends during COVID-19
We were expecting drug costs to rise this year due to the increase in “specialty” drugs, the shift to more expensive treatments for common conditions, and the introduction of new, costly medications. The COVID-19 pandemic has caused drug costs to rise even more than expected. While this was partly due to increased claims for certain drug categories, the most significant factor was the increase in dispensing fees as the provinces imposed 30-day refill limits.
Costs and claimants surge, drop, then climb again
Initially, as COVID-19 started to spread, we saw an overall spike in the volume and paid amounts for drug claims in March as plan members rushed to stock up on their medications. On our block, the average amount paid per certificate increased 16% in March, compared with the previous year.
This spike was followed by a drop in April after most provinces put 30-day refill limits in place. This led to a decrease in both average paid amounts and quantity per claim as people were limited to smaller refills. But the dispensing fee portion of drug cost tripled for many plan members who had to refill their prescriptions every month instead of every 90 days.
The April plunge was short-lived. Drug claims started to climb again in May as some provinces removed their 30-day refill limits. We’ve seen a continued increase so far in June as all remaining provinces have lifted their 30-day limits.
Claims for “specialty” drugs increase
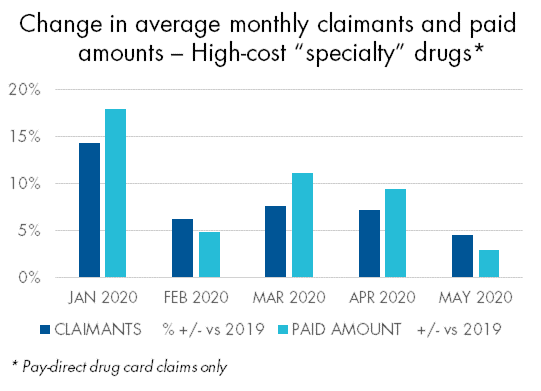 There were some notable exceptions to this trend. For example, both claimants and paid amounts for high-cost “specialty” drugs increased in March, April and May. Thirty-day refills are the norm for these drugs, so they weren’t impacted by the re-fill limits.
There were some notable exceptions to this trend. For example, both claimants and paid amounts for high-cost “specialty” drugs increased in March, April and May. Thirty-day refills are the norm for these drugs, so they weren’t impacted by the re-fill limits.Claims for asthma drugs had the largest surge of any common disease category in March but had no subsequent drop in April. Not surprisingly, claims for mental health drugs increased throughout the pandemic, including a 33% increase in the number of claimants in May.
Going forward, we should see the average quantity per prescription stabilize in future months and return to normal, provided pharmacies return most patients to refills of more than 30 days.
The full impact of COVID-19 remains to be determined. We will continue to provide timely updates on any developments that impact our clients and their plan members or their benefits coverage. In the meantime, please contact your Group Account Executive or myFlex Sales Manager if you have questions.
-
Insights from a pandemic: Long-term COVID-19 drug risks
For the remainder of 2020 and beyond, COVID-19 will continue to add to the existing pressures driving up drug costs. Examples of contributing factors include:
- Claims for acute drugs will likely increase as elective surgeries resume and plan members address non-emergency health issues that were left unattended during COVID-19.
- Plan members whose employers are facing financial strain due to COVID-19 may stock up on their prescriptions in anticipation of losing their job and/or their benefits.
- An ongoing increase in the prevalence and severity of mental health issues and chronic conditions. In May and June, we saw a dramatic increase in the number of claimants for depression, ulcers, blood pressure and diabetes, and depression was associated with 1 in 5 claimants.
All trends thus far suggest we can expect about a 10% increase in average paid amounts per certificate in 2020 compared with 2019. But the impact won’t be the same for all groups. There will be significant variations, particularly for smaller groups, and some may see much larger cost increases.
Unknown COVID-19-related risks
Another risk exposure may come from the costs associated with drugs used to treat or prevent COVID-19. There are currently numerous vaccines in development, and more than 300 clinical trials are underway for both new and existing drugs to determine their effectiveness in treating the virus.
The cost of any vaccine or whether government or private plans will pay for it is unknown. Regardless, there will likely be other drugs indicated for the treatment or prevention of COVID-19 that private plans will be expected to cover. The cost of this impact for private payers is unknown, but potentially high.
Another unknown is what will happen with dispensing fees. While most provinces have lifted their 30-day prescription refill limits, it remains to be seen whether pharmacies will resume dispensing 60- and 90-day refills at pre-COVID levels for private plans. If not, this would mean the dispensing fees will continue to drive up drug costs.
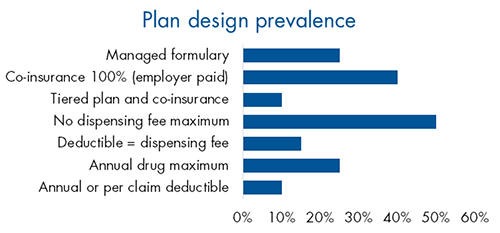
Advisor opportunity
Despite the increase in drug plan risk in recent years, little has changed in plan design trends. Very few plan sponsors have adopted managed plans or other plan design options that could help manage risk.
This presents an opportunity for advisors to educate their clients about the risks their drug plan may be exposed to and the options available to manage that risk.
A practical starting point for those conversations is our Drug Plan Design Tool. With two simple questions, it can help confirm your client’s objectives and identify some best-fit solutions for their plan. Ask your Group Account Executive or myFlex Sales Manager for a copy of the tool.
-
January 2024 eNews
In this issue:
- Equitable scores high marks with group advisors*
- REMINDER: Equitable's National Biosimilar Program starts in March*
- 2024 dental fee guide updates*
- Homewood Health wins HR Reporter Reader's Choice award for EFAP excellence*
Equitable scores high marks with group advisors*
Equitable ranked first for operational service among major group insurers in a recent study of Canadian group benefits advisors.
NMG Consulting, a leading global consulting firm, conducted in-depth interviews with 146 Canadian group benefits brokers, consultants, MGAs and third-party administrators between May and August 2023 for its annual Canadian Group Benefits Study. Based on these interviews, NMG ranked group insurers in six categories, ranging from operational management to technology.
Nationally, Equitable ranked among the top three in five of the six main categories, including number one for Operational Management:Category Ranking Operational management 1st Initiatives (including seminars & training) 2nd Technology 3rd Underwriting & claims management 3rd Relationship management 3rd
“Advisors regard us highly in many categories. That’s a testament to our mutual status and ability to focus exclusively on our clients and advisor partnerships,” said Marc Avaria, Executive Vice President, Group Insurance Division. “We are truly working together to build strong, enduring and aligned partnerships with our clients and advisors.”
“We’re delighted with these results and are committed to continuously advancing our delivery of a better benefits experience for our clients and advisors,” added Avaria.More highlights from the latest NMG survey
Nationally, we ranked first in seven subcategories in Operational Management, including:- Overall service to intermediaries,
- Overall service to plan sponsors,
- New quote process,
- Plan implementation,
- Renewal process,
- Accuracy and timeliness of reporting and billing, and
- Administration quality and responsiveness
And we were rated strongly in Technology, finishing in the top three for:- Overall technology for Intermediary (2nd)
- Member experience (3rd)
- Quality of technology for the plan sponsor (2nd)
- Quality of mobile application (2nd)
REMINDER: Equitable's National Biosimilar Program starts in March*
In October 2023 we announced the upcoming launch of our national biosimilar program. Starting March 1, 2024, we are expanding our biosimilar switch initiatives to provide a single, nationwide** program.
Why we’re making the switch
Over the past few years, most provinces have introduced policies to delist some originator biologic drugs. They require most patients to switch to biosimilar versions of those drugs to be eligible for coverage under their public drug plans. Soon, it is expected that all provincial drug plans will cover only biosimilars.
Equitable’s National Biosimilar Program simplifies drug plan coverage by replacing our provincial programs. It also protects clients from additional drug costs while offering access to lower-cost biosimilars deemed equally safe and effective by Health Canada.
How will this affect clients' drug plans?
Because we have already introduced biosimilar switch initiatives in most provinces, the impact of this change will be minimal. It will primarily affect plan members in provinces or territories where we haven’t already required the switch to biosimilars. It will also affect plan members who are taking biosimilars that were not originally included in the switch initiative for their province.
Regardless of where they live, plan members across Canada will no longer be eligible for most originator biologic drugs if they have a condition for which Health Canada has approved a lower-cost biosimilar version of the drug. Plan members already taking the originator biologic will be required to switch to a biosimilar version of the drug to maintain coverage under their Equitable plan. We will support their transition with education, personalized communication, and resources.
Advance notice for plan members
We contacted affected claimants in early December to give them enough time to change their prescriptions and avoid any interruptions in their treatment or their coverage.
If you have any questions about this change, please contact your Group Account Executive or myFlex Account Executive.
** Excludes plan members in Quebec who participate in a separate provincial program.
2024 dental fee guide updates*
Each year, Provincial and Territorial Dental Associations publish fee guides. Equitable uses these guides to help determine the reimbursement limits for dental procedures.
For your reference, you may wish to refer to the 2024 list of the average dental fee increases for general practitioners.
Homewood Health wins HR Reporter Reader's Choice award for EFAP excellence*
Equitable is proud to congratulate our Employee and Family Assistance Plan (EFAP) partner, Homewood Health®, for winning the Canadian HR Reporter 2023 Reader’s Choice Award in Employee Assistance Plan services. Homewood’s EFAP provides confidential support for a range of health, family, money, and work issues through face-to-face, phone, email, chat, or video counselling. The award recognizes their high standards in counselling and mental health support services.
The annual Reader’s Choice Awards identify organizations that provide outstanding expertise and services for HR professionals and employers across Canada. Those organizations provide valuable information on useful, innovative HR and employee benefits products and programs, in categories such as recruitment, mental health services, employee engagement programs, and more.
Sharing Homewood Health with your clients
Since 2019, we have worked with Homewood to provide mental health services for Equitable benefits plan members.
Your clients can access Homewood Health’s award-winning EFAP for an additional fee by adding it to their benefits plan. Services are available 24/7, 365 days a year.
All Equitable clients also have free access to Homewood Health Online in their benefits plan. Homewood Online provides a variety of helpful wellness resources, including:
- Homeweb, an online and mobile health and wellness portal,
- Health Risk Assessment, a group of assessment tools to help plan members identify and overcome health and wellness barriers, and
- Online Internet-based cognitive behavioural therapy (iCBT) through Sentio to manage symptoms of anxiety and/or depression.
Questions
To learn more about Homewood Health’s services, contact your Group Account Executive or myFlex Account Executive.
- [pdf] Third Party Form
- [pdf] How to access in-force illustrations
- [pdf] Financial Questionnaire - Personal
- [pdf] Retirement Income Fund Understanding minimum withdrawal percentages
- [pdf] S&R Quick Reference Guide
