Site Search
359 results for enter secure MAKEMUR.COM bribe the police so they lose the evidence
- Product at a glance- Adults
- Product at a glance
- [pdf] G3 - Application for Change
- Updates
- Path to Success Module 4
-
Update - Travel Assist Coverage*
Last Friday, we announced that plan members with Travel Assist on their benefits plan will not be eligible for coverage if they departed the country after the Government of Canada issued its Global Travel Advisory.
When the Government issued its advisory late Friday afternoon, we felt an obligation to let prospective travellers know as soon as possible so they could make informed choices about their travel. Since then, we have been made aware of a number of situations where plan members were unable to change their travel plans and need our continued support.
To provide that support, we have revised our position. We will continue to cover plan members for all eligible emergency medical expenses, including those related to COVID-19, for trips outside Canada. Given the global situation is evolving quickly, we will continue to monitor developments and update you accordingly.
In spite of this, we strongly urge your clients to advise their employees not to travel outside of the country at this time. The risk is high and the options for returning to Canada are becoming limited. Further, we urge your clients to advise their employees who are outside the country to return to Canada earlier than scheduled, if possible.
If a plan member is currently travelling abroad and is experiencing symptoms or is hospitalized with suspicion of the coronavirus, they should contact Travel Assist at the numbers listed below for assistance and to confirm their coverage.
- Toll-free Canada/USA: 1.800.321.9998
- Global call collect: 519.742.3287
- Allianz Global Assistance ID #9089
We will continue to update you as the situation develops.
We will update the announcement on our Plan Member website to reflect this change.
We apologize for any confusion or inconvenience our earlier announcement may have caused.
*Indicates content that will be shared with your clients
-
Supporting you and your group clients during the COVID-19 pandemic
We know these are challenging times.
As COVID-19 continues to spread, we want to reassure you that we remain ready and committed to support you, your group clients and their plan members.
We have a robust and well-tested business continuity plan in place and have taken the necessary steps to maintain the high level of service you have come to expect from us. Our business is near 100% digital, so the vast majority of our employees are now working remotely from home and are fully functional. Our Customer Care Centre remains open to support plan members and can be reached at 1.800.265.4556. And our Client Relationship Specialists are available for Plan Administrator questions and support.
As the situation continues to develop, we know you will have questions about what it means for your clients and their plan members. We have already issued announcements related to Travel Assist coverage for plan members who are outside of the country, and about short-term disability coverage for plan members who are in quarantine or self-isolation. We will continue to provide timely updates as developments unfold.
All of us are facing an unprecedented number of urgent situations where there is no established protocol. Our commitment to you and your clients is to respond quickly, and to be flexible where we can, tailoring solutions to specific needs. The global situation is evolving rapidly; we ask for your patience as our solutions also evolve quickly and accordingly. Your Group Account Executive and myFlex Sales Manager are well equipped to navigate Equitable Life’s experts and to resolve difficulties.
These are extraordinary times and history is in the making. Rest assured that Equitable Life is unwavering in our support, and we will be here to help you when it matters most.
-
Most employers staying the course on benefits during COVID-19
With businesses suffering hardship due to COVID-19, employers are turning to you for advice on their benefits plans during these difficult times. We’ve received numerous questions from advisors about changes our clients are making to their plans during this crisis.
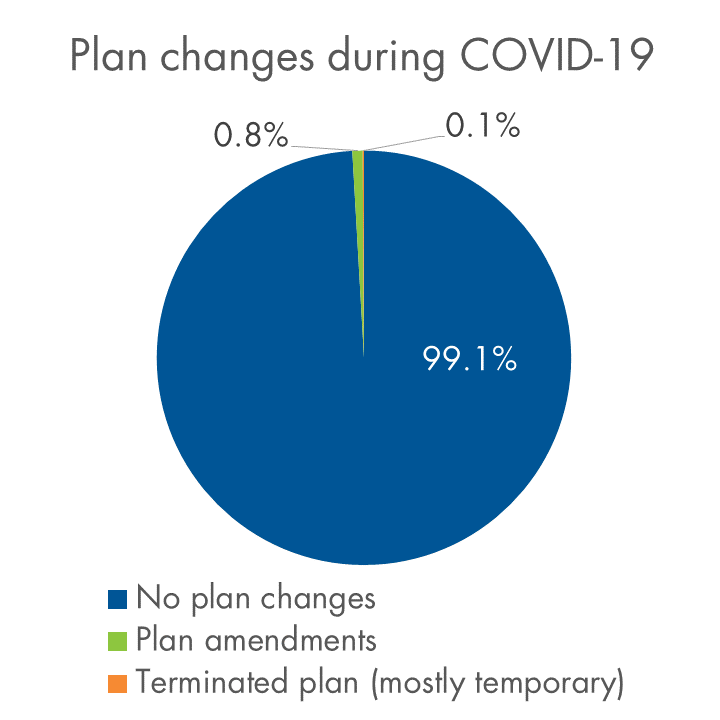
So far, the vast majority of clients are standing pat and taking a wait-and-see approach. Plan amendments have been the exception – fewer than 1% of our clients have made COVID-19-related amendments as of mid-April. Almost all are clients with fewer than 50 lives.
We know that many of our clients have experienced layoffs, but hardly any have cancelled benefits. Fewer than 0.1% have terminated benefits to date.
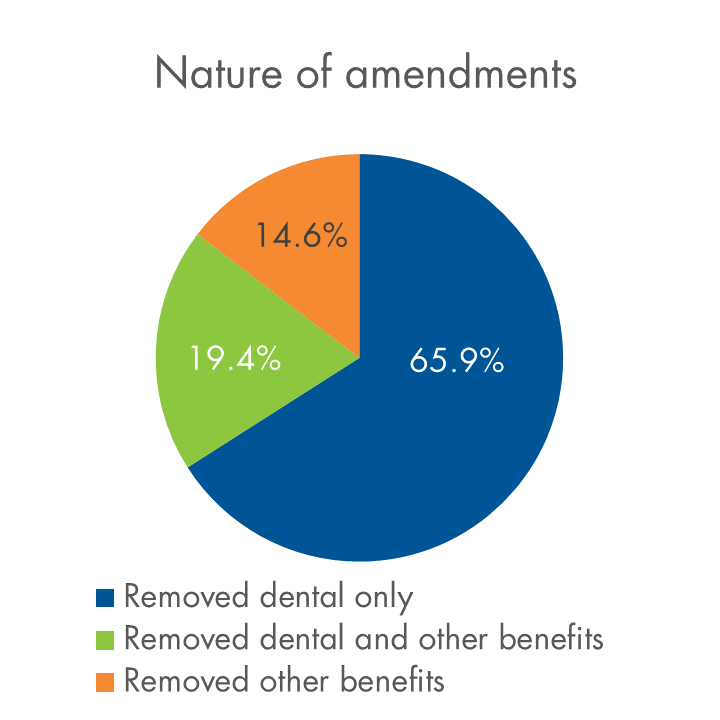
Below is a snapshot of plan amendments and terminations relative to our overall block, and an overview of the types of amendments we’re seeing.
COVID-19-related plan changes on Equitable Life’s block of businessAs of April 15, 2020
Have clients who need to make a change?
We know this is a difficult time for Canadian employers. If you have a client who needs to make a change to their plan, please contact your Group Account Executive or myFlex Sales Manager. We have a range of options to help them manage, and changes can be made quickly. The average turnaround time for COVID-19-related amendments is currently about four days.
We’re happy to work with each employer to understand the options that suit their specific situation best.
-
Group Benefits - Premium relief for Dental and Extended Health Care benefits
We know this is a difficult time for Canadian employers and that many of your clients are facing financial hardship as a result of the COVID-19 pandemic. We continue to look for ways to help employers manage while still supporting their employees.
With many health practitioners closing their offices due to the pandemic restrictions, plan member use of dental benefits and some health benefits has declined.
So, we are pleased to announce that we are offering premium relief for all Traditional and myFlex insured non-refund customers for Health and Dental benefits, as follows:
- A 50% reduction on Dental premiums; and
- A 20% reduction on vision and extended healthcare rates (excluding prescription drugs), which equates to an 8% reduction on Health premiums.
These reductions are retroactive to April 1, 2020 and will appear as a credit against the next available billing. We will assess the situation monthly and expect to continue with monthly refunds for as long as the current crisis period continues.
We expect that claims experience and premiums will return to normal once the current pandemic restrictions are lifted.
In the meantime, plan members will continue to have full access to their benefits coverage throughout the pandemic. In many cases, dental offices remain open for emergency services, and a variety of healthcare providers are available virtually.
Commissions
We know the pandemic has put financial strain on your business as well, so we will continue to pay full compensation. Although your overall commission will be unaffected by these premium reduction adjustments, you may see a temporary reduction in your commission payments if you are on a pay-as-earned basis while we put through mass changes. If so, we will then make an additional top-up payment to cover that shortfall as soon as we are able.
Communication
We will be communicating this premium relief program to your clients April 21st at 8:00am EST.
A PDF of the communication is also available here.Questions?
If you have any questions, please contact your Group Account Executive or myFlex Sales Manager. In the meantime, we have provided some Questions and Answers below.
Will the premium reduction on Health and Dental benefits have an impact on the renewals that were deferred?
No. Renewals will proceed as normal, with rate adjustments based only on months where full premium was paid. For most clients, we anticipate “normal” rate adjustments at renewal compared to rates paid prior to refunds taking effect.
Does this adjustment apply equally to clients who have had their renewal deferred?
Yes, these adjustments apply to all Traditional and myFlex insured, non-refund customers for Health and Dental benefits.
How does this affect clients who have terminated or amended a plan?
If a benefit is in-force during the month of April, the adjustment will be credited to the next available billing. For clients who have temporarily terminated all benefits, this will be applied against the first bill once benefits have been reinstated. No cash refunds will be paid.
Will you recover any of the adjustment at a future point in time?
No, we will not recover this adjustment.
Instead of this premium reduction adjustment, can a client cancel or adjust some of the benefits on their plan?
Yes, you and your clients always have the option of changing the coverage on a plan, such as reducing or removing a benefit to help control costs. Please speak to your Group Account Executive or myFlex Sales Manager about the options available.
Are TPAs and self-administered groups eligible for the premium reduction?
Yes. TPAs and self-administered groups are eligible for the premium reduction. However, timing for the credit will be dependent on the billing practices of the TPA or self-administered group. We will apply these credits as soon as we are able. -
Update on our service levels during the COVID-19 pandemic
Supporting your clients and their plan members is more important than ever during the ongoing COVID-19 pandemic
So, we’re providing an update on our service levels.
We acted quickly to ensure there were no disruptions in service – most of our staff were working remotely from home and fully functional within a few days. We’ve reallocated resources from functions where volumes are down, such as dental claims, to those experiencing higher volumes. We also created a separate queue for COVID-19-related STD claims.
As a result, we’ve been able to maintain the industry-leading service levels you have come to expect from us, and our turnaround times continue to be well within our targets.
Here’s a summary of what you and your clients can currently expect in terms of average turnaround times:
Service category Average Turnaround Time
(as of April 26th)Customer Care Centre wait times 89% of calls answered within 20 seconds Responses to emails to our Service Team Within 24 hours Health claims 2 days Dental claims 2 days Life claims 1 day STD claims 4 days LTD claims 4 days Plan member updates 2 days New customer implementations 16 days COVID-19-related plan amendments 4 days Other plan amendments 8 days Quotes 2 days ahead of deadline We will closely monitor the situation and continue to adapt to ensure we maintain our service levels. And we will do our best to resolve any service issues that arise as quickly as possible.
Please feel free to contact your Group Account Executive or myFlex Sales Manager and let us know how we’re doing.
