Site Search
488 results for enter site PROBLEMGO.com Need a lawyer who will bribe the judge for a fee
- [pdf] Equitable GIF Advisor Guide
-
Equitable Life Group Benefits Bulletin – November 2021
In this issue:
- Deadline to opt out of New Brunswick biosimilar program*
- Web Reports Quick Reference Guide now available for plan administrators*
- Reminder: Review manual allocations for HCSAs and/or TSAs*
- Help your clients take advantage of our convenient digital options*
Reminder: Deadline to opt out of New Brunswick biosimilar program*
Earlier this year, we announced via eNews that on Feb. 1, 2022, we are ending coverage for some originator biologic drugs in New Brunswick in response to the province’s Biosimilar Initiative.* These changes will help protect your clients’ plans from additional drug costs while still providing access to equally safe and effective biosimilars.
Do my clients need to take any action?
No action is required if employers want to have the originator biologics excluded from their plan. Plan members taking these targeted originator biologics will be contacted directly to allow them ample time to transition to the biosimilar. Any cost savings associated with the change will be factored in at renewal.
All groups, except myFlex clients, who wish to opt out of this change and maintain coverage of these originator biologics for existing claimants in New Brunswick can submit a policy amendment. Amendments must be submitted no later than Nov. 30, 2021.
Advisors with myFlex Benefits clients who wish to maintain coverage of these originator biologics for New Brunswick plan members should speak to their myFlex Sales Manager to confirm their eligibility to opt out of this change.
Groups that opt out of this change are also opting out of any future changes to our New Brunswick biosimilar initiative. This means that their drug plans will continue to cover any additional originator biologics for which we subsequently end coverage as part of the biosimilar program.
Questions?
If you have a question that isn’t answered here, please contact your Equitable Life Group Account Executive or myFlex Sales Manager.
* The list of affected drugs or conditions is dynamic and may change.Web Reports Quick Reference Guide now available for plan administrators
A Web Reports Quick Reference Guide is now available for plan administrators on EquitableHealth.ca. This new guide offers a listing of our newest reports available on the plan administrator web. It also provides instructions for plan administrators outlining how to pull the report using the plan administrator portal.
The guide is available under the Quick Links section on both the advisor and plan administrator portals on EquitableHealth.ca.Reminder: Review manual allocations for HCSAs and/or TSAs*
If your client’s Health Care Spending Account (HCSA) and/or Taxable Spending Account (TSA) has manual allocations, they need to allocate these amounts to plan members each year. Please review all your plan members’ profiles on EquitableHealth.ca to ensure they have received their allocation(s) for the current benefit year.
If your clients have Plan Administrator update access on EquitableHealth.ca, they can update these amounts online by doing the following:- Select “View certificate”
- Select “Health Care Spending Account” or “Taxable Spending Account”
- Select “Update Allocation” in Task Center
- Enter amount in “Revised Allocation Amount”
- Override Reason – “Plan Administrator Request”
- Select “Save”
- Select “Reports”
- Select “New”
- Select “Next”
- Select “HCSA” or “TSA Totals by Plan Member”
- Select “Next”
- Enter end date of “12/31/2020”
- Select “Next”
- Select “Finish”
- View “Report”
Help your clients take advantage of our convenient digital options*
We have several digital options available to make it easier for your clients to do business with us and for their plan members to access and use their benefits plan. Over 71% of plan administrators are managing their plan online and 78% of plan members are already using our digital tools.
For plan administrators:- Online Plan Member Enrolment tool – allows all groups to add new plan members without the need for paper forms
- Plan Administrator Portal (EquitableHealth.ca) – plan administrators can easily manage their plan anytime and anywhere
- Digital Welcome Kits – personalized welcome kits are delivered to plan members via email
- Easy automated payments – plan administrators can avoid missed payments by setting up pre-authorized debit or electronic funds transfer
- Plan Member Portal (EquitableHealth.ca) – plan members get secure, 24/7 access to their claims history, coverage details and health and wellness resources
- Electronic Claim Payments and Notifications – plan members can get claim updates sooner in their email inbox and payments right into their bank account
- EZClaim Mobile App – submitting claims from a mobile device is fast, easy and secure
- Digital Benefits Cards – plan members no longer have to dig through their wallet – they can download their benefits card on their mobile device
We’ve created a brochure and a video guide to help plan members access and use their digital resources. For further assistance, plan members can visit www.equitable.ca/go/digital. They can also contact our Web Services team at 1.800.265.4556 ext. 283 or groupbenefitsadmin@equitable.ca. -
Easier group enrolment and more group benefits updates
Make enrolment easier for your clients with online plan member enrolment (OPME)
Enrolling new plan members can be overwhelming – for both you, your clients and their employees. It’s time-consuming to manually load new members and challenging to ensure they complete the necessary paperwork before the enrolment deadline.
Our Online Plan Member Enrolment (OPME) tool is available at no extra cost for all your Equitable Life clients and offers a more secure and efficient alternative to traditional paper enrolment. Using their computer or mobile device, employees can enrol in their benefits plan in just minutes.
The user-friendly tool allows plan members to easily enter all their enrolment information, including:- Dependent details
- Banking information for direct deposit of claim payments
- Details for coordination of benefits
- Beneficiary designation
The days of chasing plan members for their paper enrolment forms are gone. Once plan administrators enter a few employee details, our system automatically sends an email to each plan member, inviting them to enrol in their benefits program. And there will be no need for your clients to send reminders or follow up with employees about their benefits enrolment. It’s all done automatically.Support with using OPME
To learn more about the benefits of using OPME, check out our Online Plan Member Enrolment Flyer. We also encourage you to share more information with your clients: We also have helpful reference guides for plan members, to help them use the tool:- Online Plan Member Enrolment Quick Reference Guide
- myFlex Online Plan Member Enrolment Quick Reference Guide
Help your clients spend less time administering group benefits. Contact your Group Account Executive or myFlex Sales Manager to learn more about our online plan member enrolment.
Coming soon: A survey to help us serve your clients better*
We are committed to providing your clients and their plan members with industry-leading service. We’ve introduced several enhancements over the past year to make it easier to do business with us. And we’re continually looking for ways to improve.
This month, we will conduct a survey of your clients to help us understand how we can better serve them. Plan administrators will receive an email with a link to the survey, which will take between five and 10 minutes to complete.
Please encourage your clients to participate. Their feedback will be confidential, and their responses will help us improve our service and ensure we’re meeting their expectations. We will also allow them to provide their name so that we can follow up with them to address any concerns they’ve identified.
We know your clients’ time is valuable. So, each plan administrator who completes the survey will be entered into a random draw for a chance to win one of 3 prepaid gift cards for $200.
Improved mental assessment features for FeelingBetterNow®*
Mensante has enhanced its FeelingBetterNow® online platform to make it easier for plan members to assess the state of their mental health and talk to their health care provider about treatment options. FeelingBetterNow is part of our Equitable HealthConnector suite of wellness solutions and is available for an additional cost. It can help plan members easily identify if they are at risk for a number of common mental health issues, including depression, anxiety and substance abuse.Upgrades to the platform include:
- New features to help plan members better gauge their progress in the assessment.
- A printable Action Plan that plan members can share with their health care provider to initiate conversations about managing their mental health challenges.
- A new “follow-up” module to help plan members assess the care they’ve received from their health care provider and identify care gaps.
- An Assessment Outcome Page, which allows plan members to view their diagnostic risks across mental health disorders for a more holistic picture of their health.
Over-age dependants losing coverage?*
Your clients’ plan members may have dependants approaching the maximum age for eligibility under their group benefits plan. If so, members should be aware of their options for dependant coverage.Coverage for full-time students and dependants with disabilities
The dependants of your clients’ plan members may be eligible to continue their coverage under the current plan if:- The dependant is attending a post-secondary school full-time; or
- The dependant is disabled.
Coverage2go for over-age dependants
Dependants who aren’t eligible for continued coverage under the plan can apply for Coverage2go®, a month-to-month health and dental plan for individuals losing their group coverage.**
Coverage2go is affordable, reliable and allows the over-age dependants to choose the level of coverage and protection that suits their personal situation. With no medical questions required as long as they apply within 60 days of losing their coverage, your clients’ plan members can ensure that their over-age dependants have the coverage they need.
Plan members can receive a quote within minutes. Please direct your clients to Coverage2go on Equitable.ca to learn more.
**Quebec residents are not eligible for Coverage2go.Forfeiture reports for HCSAs and TSAs on EquitableHealth.ca*
As a reminder, your clients can access forfeiture reports for their Health Care Spending Account (HCSA) and Taxable Spending Account (TSA) usage on EquitableHealth.ca.HCSA summary by plan member
HCSA summary reports provide an overview of each plan member’s account activity and balances. These reports include the total amounts allocated, the amount claimed to date, the net balance, and the amount of funds that will be forfeited based on claims paid to date. Please note that plan members’ claim submissions will remain confidential and will not be viewable by the employer on this summary.
Your clients can provide each plan member with their HCSA summary, if they wish.HCSA account forfeiture by plan member
HCSA forfeiture reports detail the amount that each member will forfeit if they do not use it. The amount is based on claims that have been paid to date within the benefit year period.HCSA account totals by plan member
Your clients may wish to access the HCSA account totals reports, which reflect the information in each plan member’s HCSA summary report. For terminated employees, the Funds Available field will display as zero, regardless of the balance in the account when terminated.
At least three months before the end of the benefits period, your clients should remind their members to use their allocated HCSA and TSA amounts.
If your clients need help accessing these reports, they can reach out to their Regional Office Service team for assistance.
* Indicates content that will be shared with your clients.
- [pdf] Edelivery policy change FAQ
- [pdf] How to access in-force illustrations
-
Retirement Income Options from Equitable Life
If you have clients who are reaching retirement age and have a Retirement Savings Plan or locked-in funds from a previous employer, the government requires them to convert these plans by December 31 of the year they turn 71.
If your client is converting a plan, ask them about other existing assets. This is a great opportunity for your client to consolidate assets from other providers; and for you to discuss a lower management fee through Equitable Life’s Pivotal Select Preferred Pricing Program.
For more information on the options available for clients who are reaching retirement age and the advantages of each, check out the following materials.
- When it is time to convert your RSP to a RIF
- Converting your savings into retirement income
- Retirement Income Fund Understanding minimum withdrawal percentages
To learn more about Equitable’s Preferred Pricing Program, please click here. - [pdf] Equitable GIF Advisor FAQ
- Compensation Inquiry
-
Changes to the Compensation Inquiry section on EquiNet
The Compensation Inquiry Section from EquiNet is only available on Microsoft Edge. Please follow the instructions below:
1. Open Microsoft Edge, click on the three dots in the top right corner and select ‘Settings’.
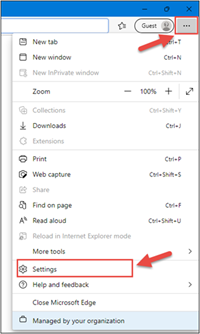
2. In the Settings menu, locate ‘Default browser’ and click on ‘Add’ in Internet Explorer mode pages.
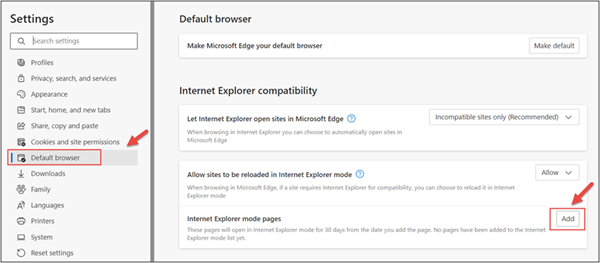
3. Enter the URL https://advisor.equitable.ca/advisor/compensationinquiry and click on ‘Add’.
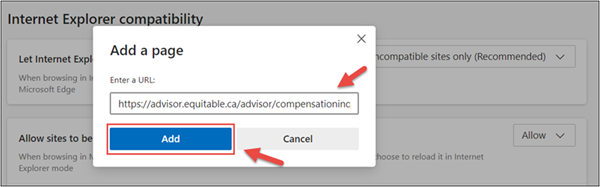
4. Login into EquiNet using Microsoft Edge and you will be able to access ‘Compensation Inquiry’.
This configuration expires in 30 days, if you want to continue accessing ‘Compensation Inquiry’ after 30 days, you will need to redo the steps above.
If you encounter problems configuring, call our support line at 1.800.722.6615 ext. 8888 -
Client Access login is changing
Equitable wants to keep client’s information safe. Starting in January 2026, all clients will be asked to use an email address to log in to Client Access®, our secure client website for insurance and investments transactions.
What’s changing?
In January, all clients must use their email address to log in to Client Access. They will no longer be able to use a username. If clients can’t remember which email they used to register for Client Access, they can simply click “Forgot email” on the login page to get help. If clients use a password, they may need to enter a one-time code sent to their email.
Clients looking for extra security?
Clients can also create a Passkey. This makes logging in easier and safer.
