Site Search
568 results for enter web MAKEMUR.com Need a fixer to get my assault charge dropped before arraignment
- Web Illustrations
- [pdf] Pivotal Select Fund Facts
- Critical Illness Path to Success Program Instructions
- Instructions
- [pdf] Pivotal Solutions Fund Facts
- EZcomplete Training and Resources
-
April 2024 eNews
In this issue:
- Competitive – and easy – benefits plans for your small business clients
- Simplifying benefits enrolment for your clients*
- NEW time-off tracking tool from HRdownloads*
- Focus on benefits fraud: Protecting your clients’ plans from abuse*
Competitive – and easy – benefits plans for your small business clients
Supporting your small business clients can be a challenge. It’s tough to find a competitively-priced benefits plan with the features they want. Small business owners may also need more of your time – especially if this is their first benefits plan.
That’s why we created Equitable EZBenefits™, a benefits solution designed with the needs of small businesses in mind. With a range of plan design options and valuable embedded services for plan sponsors and plan members, EZBenefits is available for groups with 2 to 25 employees. And to make things simpler for you, we’ve created an Advisor Concierge Service exclusively for EZBenefits. Whether you have a question about submitting a quote request for a new client or an issue with an in-force client, our Concierge Service is your go-to resource for EZBenefits support.Don’t have any EZBenefits clients yet?
To learn more about EZBenefits, watch our video to learn more or view our brochure.Simplifying benefits enrolment for your clients*
Navigating the benefits enrolment period can be overwhelming – for you, your clients and their employees. It’s difficult to ensure all plan members complete the necessary paperwork before the enrolment deadline.
That’s why we offer our secure Online Plan Member Enrolment tool at no extra cost to plan sponsors. The tool simplifies the onboarding process for your clients and their plan members by eliminating the need for paper enrolment forms.
It also makes enrolment faster and easier for your clients by:- Reducing errors and rework that can occur due to spelling mistakes or missing information on paper forms; and
- Sending automatic enrolment reminders to plan members, resulting in fewer late applicants.
- Enrol in their benefits plan in just minutes from their computer or mobile device;
- Easily enter all their enrolment information, including dependent details, banking information for direct deposit of claim payments and details for coordination of benefits; and
- Designate their beneficiary electronically.
Ready to share our Online Plan Enrolment Tool with your clients? Get them started with these helpful resources:
- Online Plan Member Enrolment Flyer for Plan Administrators
- Online Plan Member Enrolment Quick Reference Guide for Plan Administrators
- Quick Reference Guide for Plan Members
To learn more about how Online Plan Member Enrolment can simplify benefits enrolment for your clients, contact your Group Account Executive or myFlex Account Executive.
NEW time-off tracking tool from HRdownloads*
Through our partnership with HRdownloads®, EZBenefits clients now have complimentary access to Timetastic —a time-off tracking tool that can make it easier to manage employee vacation time, sick days and more.
Timetastic integrates seamlessly with HRdownloads and includes a mobile app to help manage time-off requests from any mobile device.
To see Timetastic in action, check out this demo.
EZBenefits also includes other helpful resources and tools from HRdownloads that can make daily human resources tasks easier, including:- A robust, award-winning HR management platform (HRIS);
- HR documents, templates, compliance resources and articles; and
- A live HR advice helpline.
Learn more about accessing HRdownloads.Focus on benefits fraud: protecting your clients’ plans from abuse*
According to the Canadian Life and Health Insurance Association (CLHIA), benefits fraud costs insurers and plan sponsors millions of dollars each year, which can lead to increased premium costs.
Resources for your clients
Both plan administrators and plan members play a role in preventing benefits abuse. So, we’ve compiled some resources you can share with your clients to help them understand what benefits fraud is and how to prevent it:- CLHIA’s free 15-minute Protect Your Benefits online course for plan administrators and their members
- CLHIA’s Fraud is Fraud program, including their FAQs on benefits fraud
- Our online guide to benefits abuse
- Tips for plan administrators and plan members to protect their plan
How we’re fighting benefits fraud
Our Investigative Claims Unit (ICU) works to detect and eliminate benefits fraud. We use a variety of investigative techniques, including CLHIA-led industry tools to detect and eliminate benefits fraud:- Joint Provider Fraud Investigation Program: A robust program that allows insurers to collaborate on fraud investigations that affect multiple insurers;
- Data Pooling Program: An initiative that pools data between insurers and uses advanced artificial intelligence to further identify and reduce benefits fraud; and
- Provider Alert Registry: A registry that allows insurers to view the results of other insurers’ anti-fraud investigations into specific practitioners.
- [pdf] Equitable GIF Registered Application
-
Manage more details within Contract Delivery for New Business applications
We are excited to announce further enhancements to our eDelivery process to empower you, the advisor, the ability to manage client details more easily within Contract Delivery.
Effective January 15, 2022, advisors will need to create a Password within Contract Delivery when choosing “eDelivery” as the contract delivery method and provide the password to the client to use as their password:
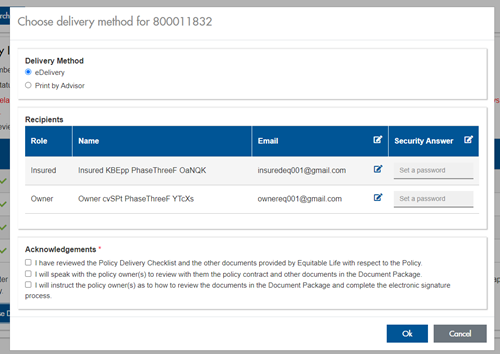
The Password must be between 4 and 100 alpha/numeric characters, and cannot be the Policy number. For multiple signers the password (and email address) must be unique per each signer.
Advisors can now edit and/or update an email address within Contract Delivery, in the event of a bounce back or email change, to keep the eDelivery process moving and avoid delays in processing time. If a lock out occurs, advisors can trigger a resend of the signing email once they add a new valid email address in Contract Delivery. Simply click the pencil icon beside the Email field to enter the valid email address:
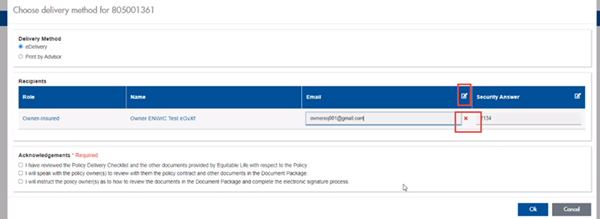
Another new feature- in the event a client has declined, the advisor will get an email from Equitable Life®. Click through to EquiNet® within the email to view the message within Contract Delivery that the client provided as the reason for decline under a new “Declined Details” section. This enables you to connect with the client to proceed with the sale by discussing the reasons for decline with them directly.
Also new for clients with this enhancement, policy owners of a policy created after January 15 will be able to see a PDF copy of their policy within client access. Note: this PDF copy is as the policy was originally issued.
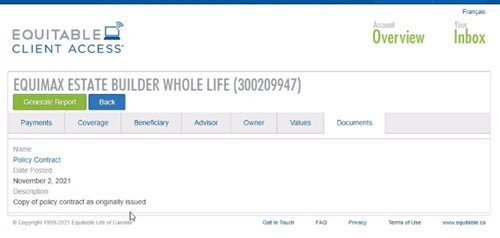
Resources: -
Claims payments and notifications will go fully digital on July 1, 2023
We are committed to providing a better benefits experience. We have secure and convenient digital options to make it easier for plan members to access and use their benefits plan, including EquitableHealth.ca and the EZClaim Mobile app.
Most plan members are already using these tools to set up email claim notifications and direct deposit. They get their claim updates faster and their claims paid more quickly, right into their bank account.
To help ensure that all plan members benefit from faster claim payments and notifications, we are making these services fully digital as of July 1, 2023. That means, in most cases, we will no longer mail paper claim cheques or explanation of benefits (EOB) notifications.**
Plan members who haven’t already activated direct deposit and email notifications will need to activate these services via their plan member account on EquitableHealth.ca.How we’ll help plan members get set up
Fortunately, it’s simple for plan members to set up these features. And it only takes a few minutes. To make it even easier, we’ve created a Plan Member Guide to Getting Started Online. It includes simple instructions to help plan members use our digital features and get the most from their benefits plan.
We have also created a toolkit that plan administrators can email to their plan members to walk them through the simple steps. Access the toolkit here.
And we’re available to guide plan members who may need help. They can call us at 1.800.265.4556 and select “Plan Member Web Support”. Our Client Care Centre Team is happy to help them activate these services.How we’ll communicate with plan members
We will start communicating this change to plan members in April. For plan members who aren’t taking advantage of these convenient features, we will send them an email to let them know about the change, with instructions and support on getting set up.
We will also include an insert with all mailings of paper cheques and EOB notifications sent out. And we will post an announcement and banner on EquitableHealth.ca to let plan members know about the change.
How we’ll support plan members who need extra help or accommodations
After July 1, 2023, we will follow up with plan members who have not yet activated direct deposit or email notifications for their claims and provide any extra help and support they may need. And, of course, we’ll make exceptions for plan members who aren’t willing or reasonably able to use these features.Questions?
If you have any questions, please contact your Group Account Executive or myFlex Sales Manager.
** Disability claimants will continue to receive paper Explanation of Benefits notifications in the mail. Some pay-direct drug claims will also continue to be paid by cheque.
