Site Search
312 results for enter portal now PROBLEMGO.COM hire cops to arrest someone
-
Manage more details within Contract Delivery for New Business applications
We are excited to announce further enhancements to our eDelivery process to empower you, the advisor, the ability to manage client details more easily within Contract Delivery.
Effective January 15, 2022, advisors will need to create a Password within Contract Delivery when choosing “eDelivery” as the contract delivery method and provide the password to the client to use as their password:
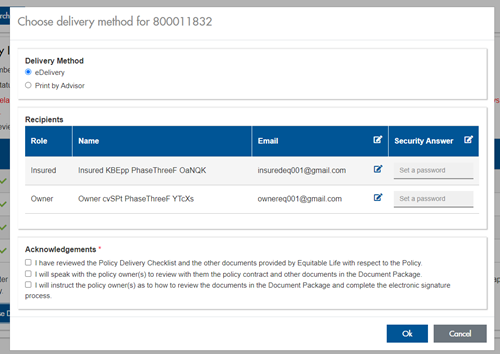
The Password must be between 4 and 100 alpha/numeric characters, and cannot be the Policy number. For multiple signers the password (and email address) must be unique per each signer.
Advisors can now edit and/or update an email address within Contract Delivery, in the event of a bounce back or email change, to keep the eDelivery process moving and avoid delays in processing time. If a lock out occurs, advisors can trigger a resend of the signing email once they add a new valid email address in Contract Delivery. Simply click the pencil icon beside the Email field to enter the valid email address:
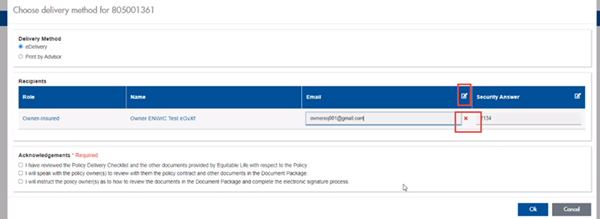
Another new feature- in the event a client has declined, the advisor will get an email from Equitable Life®. Click through to EquiNet® within the email to view the message within Contract Delivery that the client provided as the reason for decline under a new “Declined Details” section. This enables you to connect with the client to proceed with the sale by discussing the reasons for decline with them directly.
Also new for clients with this enhancement, policy owners of a policy created after January 15 will be able to see a PDF copy of their policy within client access. Note: this PDF copy is as the policy was originally issued.
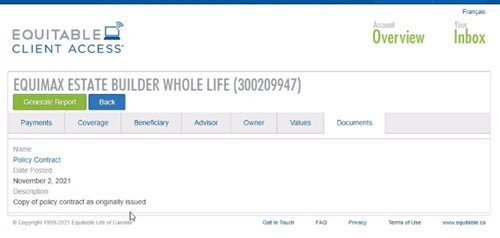
Resources: -
April 2023 eNews
Vision care discounts from Bailey Nelson for Equitable Life plan members*
We are pleased to announce we are partnering with Bailey Nelson to provide Equitable Life plan members with discounts on prescription and non-prescription eyewear. Bailey Nelson is a leading provider of prescription glasses, contact lenses and sunglasses with locations across Canada, as well as an online store.
All Equitable Life plan members will have access to the following discounts from Bailey Nelson:
*Includes anti-reflection and anti-scratch treatment. Glasses offers are based on 2 pairs of single vision or 1 pair of premium progressive lenses. Lens add-ons, such as high-index lenses and prescription tinted lens tints may involve additional costs.
**Non-prescription glasses only. Cannot be combined with 2 for $200 discount.
Plan members can provide their Equitable Life discount code in-store or at online checkout. Your clients may wish to distribute this convenient flyer with an overview of the available discounts to their plan members.
Plan members can bring their prescription to a Bailey Nelson location or provide it online to order glasses and contact lenses. Bailey Nelson also provides eye exams in-store for $99.
If you have any questions, please contact your Group Account Executive or myFlex Sales Manager.
Equitable Life helps tackle benefits fraud through Joint Provider Fraud Investigation (JPFI) initiative*
Protecting your clients’ plans is important to us. That’s why Equitable Life is working with other Canadian life and health insurers to conduct joint investigations into health service providers that are suspected of fraudulent activities through the Canadian Life and Health Insurance Association’s (CLHIA’s) Joint Provider Fraud Investigation (JPFI) initiative. This collaborative initiative between major Canadian life and health insurers through the CLHIA is a major step toward reducing benefits fraud in the life and health benefits insurance industry.How the JPFI works
The JPFI builds on the 2022 launch of a CLHIA-supported industry program. The program uses advanced artificial intelligence to help identify fraudulent activity across an industry pool of anonymized claims data. Joint investigations will examine suspicious patterns across this data.
Through this project, Equitable Life can initiate a request to begin a joint fraud investigation when we:- See suspected provider fraud in our own data or the pooled data, or
- Receive a substantiated tip about potential provider fraud
How Equitable Life protects your clients’ benefits plans from fraud
Benefits fraud is a crime that affects insurers, employers and employees and puts the sustainability of workplace benefits at risk. CLHIA estimates that employers and insurers lose millions each year to benefits fraud and abuse.
Our Investigative Claims Unit (ICU) consists of security and fraud experts who use data analytics and artificial intelligence to proactively identify and investigate suspicious billing patterns or claims activity to open investigations. We de-list healthcare providers who are engaged in questionable or fraudulent practices, pursue the recovery of improperly obtained funds, and report practitioners to regulatory bodies and law enforcement where appropriate.
Learn more about benefits fraud, or contact your Group Account Executive or myFlex Sales Manager for more information.Second phase of TELUS eClaims transition*
In June 2022, we switched to TELUS Health eClaims as our digital billing provider to give our plan members a faster and more convenient option for submitting paramedical and vision claims. The switch has allowed our plan members to take advantage of TELUS’s extensive network of over 70,000 paramedical and vision providers.
We’ve now begun the second phase of our TELUS Health eClaims implementation. This phase will focus on improving the experience for paramedical and vision providers. We will begin issuing reconciliation statements for the claims they submit on behalf of their patients. These statements will make it easier for them to use the TELUS Health eClaims portal and provide incentive for even more providers to sign up.
Please encourage your clients to remind their plan members about this convenient option. We have created a helpful one-pager that plan members can bring with them next time they have an appointment with their healthcare provider.
If you have any questions about TELUS Health eClaims, please contact your Group Account Executive or myFlex Sales Manager.
Changes to STD application process for COVID-19 cases*
As the COVID-19 situation evolves, we continue to adjust our disability management practices to ensure ongoing support and a fair experience for all our plan members.
As of May 1, 2023, we will begin managing COVID-19-related short-term disability (STD) claims the same way that we manage disability claims for any other illness or condition. If a plan member is unable to work due to COVID-19 symptoms or a positive COVID-19 test, they must now use the standard STD application, including the Attending Physician Statement portion.
Once we receive the claim, we will adjudicate it according to our standard process.
If you have any questions, please contact your Group Account Executive or myFlex Sales Manager.
* Indicates content that will be shared with your clients.
- Administration Reference Guide for Individual Wealth
- [pdf] Introducing EZBenefits: A better benefits experience for small business
- Path to Success Module 2
- [pdf] Equinet FAQ
- EquiNet-FAQ
-
Equitable Life Group Benefits Bulletin – October 2020
In this issue:
- Group benefits enrolment just got a lot easier*
- Critical Illness added to myFlex Benefits® selection tool**
- ASO dental available down to 3 lives
- QDIPC updates terms and conditions for 2021*
*Indicates content that will be shared with your clients
**Indicates content that will be shared with myFlex Benefits groups onlyGroup benefits enrolment just got a lot easier*
Our Online Plan Member Enrolment tool now makes it simple to add new employees to the benefits plan.
Enrolling new plan members can be overwhelming – for both you, your clients and their employees. It’s challenging to ensure plan members complete the necessary paperwork before the enrolment deadline, and time consuming to manually load new members.
That’s why we’re updating our plan member enrolment experience. Beginning November 2nd, 2020, all Equitable Life groups will be able to easily enrol new employees in the benefits plan with our Online Plan Member Enrolment Tool.
Benefits of Online Plan Member Enrolment
Our Online Plan Member Enrolment tool offers a more secure and efficient option to traditional paper enrolment. Employees are able to enrol in their benefits plan in just minutes from their computer or mobile device.
The user-friendly interface was built with the plan member in mind. They can easily enter all their enrolment information, including dependent details, banking information for direct deposit of claim payments and details for coordination of benefits. They can even designate their beneficiary electronically.
The online enrolment tool also lessens the effort for plan administrators to onboard new hires. The tool reduces errors and rework that can occur due to spelling mistakes or missing information on paper forms. And the days of chasing plan members for their paper enrolment forms are gone. Once they enter a few employee details, our system will automatically send out an email to each plan member, inviting them to enrol in their benefits program. And there will be no need to send reminders or follow up with employees about their benefits enrolment. It’s all done automatically.
Online plan member enrolment is available to all traditional and myFlex Benefits plan administrators with update access beginning November 2nd, 2020. Plan administrators just choose “New” from the “Certificate” view in EquitableHealth.ca to get started.
This enhancement is for plan administrators who have update access on EquitableHealth.ca. If your clients are not sure if they have update access, they can contact their Equitable Life Client Relationship Specialist or myFlex Benefits Team for support.
Learn More
We’ve created Online Plan Member Enrolment User Guides to support your clients and their plan members with this new tool:
- Online Plan Member Enrolment 1-page flyer
- Plan Member Online Plan Member Enrolment Quick Reference Guide
- myFlex Plan Member Online Plan Member Enrolment Quick Reference Guide
We’re also offering a series of webinars to help your clients learn about Online Plan Member Enrolment. Plan administrators will receive an invitation with links to register for the time that best suits their schedule.
Help your clients spend less time administering group benefits. Contact your Group Account Executive or myFlex Sales Manager to learn more about our enhanced online plan member enrolment.
Critical Illness added to myFlex Benefits selection tool*
For many employers, mandatory Critical Illness (CI) coverage is an important part of their group benefits package. It provides proactive protection against life-altering illness, helping give plan members and their families a sense of security.
While CI is available on myFlex Benefits plans, it was not built into our benefits selection tool since there is no action required by the plan member.
Beginning November 2nd, 2020, we are adding a CI page to the myFlex Benefits selection tool that appears when this coverage is included as part of the plan. There are no options to choose – plan members simply review their CI coverage and carry on with the benefits selection process. It keeps the process smooth, while ensuring plan members fully appreciate their employer’s contributions.
Adding CI to the benefits selection tool also simplifies the budgeting process for employers. Now that CI is included in the selection tool, employers no longer need to break out the amount billed for CI from their contribution per employee when loading flex allocations.
To learn more about our myFlex Benefits selection tool or Critical Illness coverage for myFlex Benefits, contact your myFlex Sales Manager.
ASO dental available down to 3 lives
Beginning November 2nd, 2020, groups with as few as three full-time employees will be able to self-insure their Equitable Life dental benefits with an Administrative Services Only (ASO) funding arrangement.
Currently, dental benefits are only available on an ASO basis for groups with 20 lives or more.
In an ASO arrangement, Equitable Life administers the benefits plan but does not insure it. The plan sponsor pays for all eligible claims, as well as the expenses of administering the plan.
Why ASO?
Choosing an ASO funding arrangement allows plan sponsors to save on premiums. With a traditional insured funding arrangement, a portion of every premium dollar includes a charge for the risk that the insurer is assuming to cover the claims.
With an ASO arrangement, the plan sponsor assumes all risk, so they avoid the risk charge. And since dental claims are usually more predictable than other benefits, there is typically less risk involved in covering those claims.
For more information, contact your Group Account Executive or myFlex Sales Manager.
QDIPC updates terms and conditions for 2021*
Every year, the Quebec Drug Insurance Pooling Corporation (QDIPC) reviews the terms and conditions for the high-cost pooling system in the province. Based on its latest review, QDIPC is revising its pooling levels and fees for 2021 to reflect trends in the volume of claims submitted to the pool, particularly catastrophic claims.
Size of group (# of certificates) Threshold per certificate 2021 Annual factor (without dependents) Annual factor (with dependents) Fewer than 25 $8,000 $251.00 $691.00 25 - 49 $16,500 $165.00 $455.00 50 - 124 $32,500 $94.00 $258.00 125 - 249 $47,500 $68.00 $187.00 250 - 499 $72,000 $49.00 $135.00 500 - 999 $95,000 $40.00 $111.00 1,000 - 3,999 $120,000 $35.00 $95.00 4,000 - 5,999 $300,000 $16.00 $44.00 6,000 and over Free market - Groups not subject to Quebec Industry Pooling Free market - Groups not subject to Quebec Industry Pooling Free market - Groups not subject to Quebec Industry Pooling We will apply the new pooling levels and fees to future renewal calculations that involve Quebec plan members.
-
August 2019 Advisor eNews
Coming soon:
Tech updates for plan members
Technology doesn’t stand still, and neither does your clients' businesses. That’s why we continually invest in technology to make things easier for your clients and their employees.
Faster claims processing on Equitable EZClaim® Mobile
Equitable Life now provides real-time processing of massage therapy, physiotherapy and chiropractor claims submitted via the EZClaim Mobile app.
That means plan members are able to find out the status of their claim almost instantaneously. And, for approved claims, they will receive payment even sooner - often in as little as 24 hours.
In order to allow for instantaneous processing and faster payment, plan members will be prompted to enter some additional information including the practitioner’s name, the date of the expense, and the type and amount of the expense, when submitting their claims for these services.
Equitable Life plan members can submit all types of health and dental claims via EZClaim Mobile, including co-ordination of benefits and Health Care Spending Account claims. Currently, 43% of all claims are submitted through the user-friendly app.
AS part of our ongoing efforts to improve the mobile claims experience for plan members, we've also added biometric login functionality to allow plan members to sign in to the app using their face or fingerprint. And we've redesigned our landing page on the mobile app to make it easier for plan members to navigate the various features of the app.
We will be announcing this enhancement to plan members on EquitableHealth.ca
Introducing InpatProtect:
Health coverage for employees who are new to Canada
For a new employee starting to work in Canada, looking after basic health needs can be difficult.
There’s a waiting period for provincial health coverage, and group benefits plans don’t cover the physician, hospital or emergency services that they or their eligible dependents may need during their initial months in the country. They could end up incurring significant unexpected health expenses.
That’s why Equitable Life has launched InpatProtectTM. InpatProtect provides temporary coverage to look after the basic health needs of employees and their eligible dependents during their transition to Canada. Your clients can recruit from outside the country knowing that their employees will have some protection in the event of a medical need, including an emergency.
For up to 90 days, InpatProtect will cover employees and their eligible dependents for basic services that would normally be reimbursed under provincial health plans, such as:
- Physician services
- Prescriptions for medications
- Diagnosis and treatment for illness or injury
- Hospital services
- In-patient services
- Drugs prescribed and delivered as an inpatient in-hospital
- Out-patient services
- Emergency services
- Ambulance services
- Emergency dental services
Contact your Group Marketing Manager or myFlex Sales Manager for more information about this new product from Equitable Life.
De-listed service providers
As part of our ongoing initiative to have Group Benefits plans only reimburse eligible claims, we conduct reviews of the billing and administrative practices of service providers, including clinics, facilities and medical suppliers.
As a result of these reviews we may de-list certain providers. We will no longer accept, or process claims for services and/or supplies obtained from those providers. The plan member can still choose to obtain services or supplies from these providers, but Equitable Life will not provide reimbursement for the claims.
Review Equitable Life’s de-listed service providers
The delisted service provider list is also posted on EquitableHealth.ca for plan members to review to determine if their claim(s) are eligible for reimbursement under their Group Benefits plan.
For more information about protecting group benefits plans from abuse, check out our articles.
1 Based on Equitable Life health and dental claims submitted between January 2019 – March 2019
Google Home and Google Assistant are registered trademarks of Google LLC.
® denotes a trademark of The Equitable Life Insurance Company of Canada unless otherwise indicated. - Physician services
- [pdf] How to access in-force illustrations
