Site Search
354 results for view portal now MAKEMUR.com bribe a judge for a lighter sentence in court
- [pdf] Third Party Form
-
Roll out the red carpet for a refreshed Term!
We are pleased to announce that updates to our Term life insurance solution are now live! We believe that Term life insurance can deliver value to clients at every stage of their life journeys. Be it at renewal or at conversion, Term is a flexible and affordable life insurance solution for clients today and into tomorrow.
On February 3rd, 2024, we refreshed our Term life insurance solution. Some of the existing and new updates with our Term offering include:
● More targeted, competitive pricing,
● Benefits re-aligned under the KIND™ program,
● Yearly renewals. After the initial term of level premiums, Term life insurance will now renew yearly with premiums gradually increasing each year. This will help clients keep their Term protection longer without large premium increases.
With these updates and more, our Term solution doesn’t just “do the job,” it’s what clients want!
Visit our splash page and watch our informative video to learn more and start selling today!
.png)


View our Transition Rules for all the details on processing your applications.
We’ve also updated our illustration tool:
● New Desktop illustration software
Want to learn more?
Contact your Equitable wholesaler anytime!
® or ™ denotes a trademark of The Equitable Life Insurance Company of Canada. - Sales Illustrations
- Total Cost Reporting: understanding what's coming next
-
Equitable Life Group Benefits Bulletin – November 2020
In this issue:
- Telemedicine now included in Travel Assist*
- Take advantage of our convenient digital options*
- 2021 changes to Maximum Insurable Earnings, Maximum Weekly Insurable Earnings and Short Term Disability Benefit*
*Indicates content that will be shared with your clients
Telemedicine now included in Travel Assist*
Medical emergencies can be particularly stressful while travelling. Making your way to a medical facility can be a struggle. And once you get there, you could face long wait times, language barriers or even the risk of COVID-19 infection.
That’s why Allianz Global Assistance®, our Travel Assist provider, is adding two new virtual care options to provide plan members with timely and appropriate medical support.
As always, when a travel medical emergency strikes, plan members call Allianz for assistance. During the intake process plan members will be guided through a series of questions to triage their unique medical situation. Options for care now include two different virtual care services:
- TeleConsultation – Video and chat consultation with a locally licensed physician. This physician can diagnose simple medical conditions and provide a prescription. Available across Canada and in some high travel states in the United States.
- TeleAdvice – Video and chat consultation for situations which are not likely to require a prescription. The physician can diagnose simple medical conditions and provide medical guidance.
Plan members who use virtual care may benefit from:
- Reduced wait times;
- Care from the comfort of their current location;
- Reduced language barriers;
- No need to arrange transportation to a medical facility;
- Reduced impact on travel itinerary; and
- Reduced risk of exposure.
Both TeleConsultation and TeleAdvice will be available for all Equitable Life plan members beginning January 1st, 2021. There is no additional cost, no changes required to your client’s plans, and no change to the way plan members contact Allianz in the event of a travel medical emergency.
This PDF plan member update will also be included in the eNews to plan administrators.
If you have any questions about these new features, please contact your Equitable Life Group Account Executive or myFlex Sales Manager.
Allianz Global Assistance is a registered business name of AZGA Service Canada Inc. and AZGA Insurance Agency Canada Ltd.
Help your clients take advantage of our convenient digital options*
During this time of physical distancing, people are looking for ways to interact with their providers virtually. We recently enhanced our Online Plan Member Enrolment tool, allowing all groups to add new plan members without the need for paper forms.
Did you know, we have several other digital options available to make it easier for your clients to do business with us and for their plan members to access and use their benefits plan? Over 71% of plan administrators are managing their plan online and 78% of plan members are already using our digital tools.
For plan administrators:
- Plan Administrator Portal (EquitableHealth.ca) – plan administrators can easily manage their plan anytime and anywhere
- Digital Welcome Kits – personalized welcome kits are delivered to plan members via email
- Easy automated payments – plan administrators can avoid missed payments by setting up pre-authorized debit or electronic funds transfer
For plan members:
- Plan Member Portal (EquitableHealth.ca) – plan members get secure, 24/7 access to their claims history, coverage details and health and wellness resources
- Electronic Claim Payments and Notifications – plan members can get claim updates sooner in their email inbox and payments right into their bank account
- EZClaim Mobile App – submitting claims from a mobile device is fast, easy and secure
- Digital Benefits Cards – plan members no longer have to dig through their wallet – they can download their benefits card on their mobile device
Learn more about how we’re making it easier for your clients to do business with us
2021 changes to Maximum Insurable Earnings, Maximum Weekly Insurable Earnings and Short Term Disability Benefit*
The Canada Employment Insurance Commission and Canada Revenue Agency have announced the 2021 changes to Maximum Insurable Earnings, and premiums for employment insurance. These changes take effect January 1st, 2021.
Maximum Insurable Earnings (MIE)
The MIE will increase from $54,200 to $56,300.
Maximum Weekly Insurable Earnings (MWIE)
The MWIE will increase from $1,042 to $1,083.
EI Benefit (55% of the MWIE, rounded to the nearest dollar)
EI benefit will increase from $573 to $595
Information for Plan sponsors
If your client’s Group Policy with Equitable Life includes a Short Term Disability (STD) benefit which is tied to the EI MWIE, and at least one classification of employees has less than a $595 maximum:
- To comply with the provisions of their policy, their STD benefit will be revised with the maximums updated based on the percentage of EI MEIW shown in their policy.
- The additional premium for any increase from their previous STD amounts and new STD amounts will be show on their January 2021 Group Insurance Billing (as applicable).
If their STD maximum is currently higher than $595 or based on a flat amount (not based on a percentage or regular earnings):
- No change will be made to their plan unless otherwise directed.
If your clients wish to provide direction regarding revising their STD maximum, or have questions about the process, they can email Kari Gough, Manager, Group Quotes and Issue.
*Indicates content that will be shared with your clients
-
April 2023 eNews
Vision care discounts from Bailey Nelson for Equitable Life plan members*
We are pleased to announce we are partnering with Bailey Nelson to provide Equitable Life plan members with discounts on prescription and non-prescription eyewear. Bailey Nelson is a leading provider of prescription glasses, contact lenses and sunglasses with locations across Canada, as well as an online store.
All Equitable Life plan members will have access to the following discounts from Bailey Nelson:
*Includes anti-reflection and anti-scratch treatment. Glasses offers are based on 2 pairs of single vision or 1 pair of premium progressive lenses. Lens add-ons, such as high-index lenses and prescription tinted lens tints may involve additional costs.
**Non-prescription glasses only. Cannot be combined with 2 for $200 discount.
Plan members can provide their Equitable Life discount code in-store or at online checkout. Your clients may wish to distribute this convenient flyer with an overview of the available discounts to their plan members.
Plan members can bring their prescription to a Bailey Nelson location or provide it online to order glasses and contact lenses. Bailey Nelson also provides eye exams in-store for $99.
If you have any questions, please contact your Group Account Executive or myFlex Sales Manager.
Equitable Life helps tackle benefits fraud through Joint Provider Fraud Investigation (JPFI) initiative*
Protecting your clients’ plans is important to us. That’s why Equitable Life is working with other Canadian life and health insurers to conduct joint investigations into health service providers that are suspected of fraudulent activities through the Canadian Life and Health Insurance Association’s (CLHIA’s) Joint Provider Fraud Investigation (JPFI) initiative. This collaborative initiative between major Canadian life and health insurers through the CLHIA is a major step toward reducing benefits fraud in the life and health benefits insurance industry.How the JPFI works
The JPFI builds on the 2022 launch of a CLHIA-supported industry program. The program uses advanced artificial intelligence to help identify fraudulent activity across an industry pool of anonymized claims data. Joint investigations will examine suspicious patterns across this data.
Through this project, Equitable Life can initiate a request to begin a joint fraud investigation when we:- See suspected provider fraud in our own data or the pooled data, or
- Receive a substantiated tip about potential provider fraud
How Equitable Life protects your clients’ benefits plans from fraud
Benefits fraud is a crime that affects insurers, employers and employees and puts the sustainability of workplace benefits at risk. CLHIA estimates that employers and insurers lose millions each year to benefits fraud and abuse.
Our Investigative Claims Unit (ICU) consists of security and fraud experts who use data analytics and artificial intelligence to proactively identify and investigate suspicious billing patterns or claims activity to open investigations. We de-list healthcare providers who are engaged in questionable or fraudulent practices, pursue the recovery of improperly obtained funds, and report practitioners to regulatory bodies and law enforcement where appropriate.
Learn more about benefits fraud, or contact your Group Account Executive or myFlex Sales Manager for more information.Second phase of TELUS eClaims transition*
In June 2022, we switched to TELUS Health eClaims as our digital billing provider to give our plan members a faster and more convenient option for submitting paramedical and vision claims. The switch has allowed our plan members to take advantage of TELUS’s extensive network of over 70,000 paramedical and vision providers.
We’ve now begun the second phase of our TELUS Health eClaims implementation. This phase will focus on improving the experience for paramedical and vision providers. We will begin issuing reconciliation statements for the claims they submit on behalf of their patients. These statements will make it easier for them to use the TELUS Health eClaims portal and provide incentive for even more providers to sign up.
Please encourage your clients to remind their plan members about this convenient option. We have created a helpful one-pager that plan members can bring with them next time they have an appointment with their healthcare provider.
If you have any questions about TELUS Health eClaims, please contact your Group Account Executive or myFlex Sales Manager.
Changes to STD application process for COVID-19 cases*
As the COVID-19 situation evolves, we continue to adjust our disability management practices to ensure ongoing support and a fair experience for all our plan members.
As of May 1, 2023, we will begin managing COVID-19-related short-term disability (STD) claims the same way that we manage disability claims for any other illness or condition. If a plan member is unable to work due to COVID-19 symptoms or a positive COVID-19 test, they must now use the standard STD application, including the Attending Physician Statement portion.
Once we receive the claim, we will adjudicate it according to our standard process.
If you have any questions, please contact your Group Account Executive or myFlex Sales Manager.
* Indicates content that will be shared with your clients.
-
Enhancements to ID Verification and Business Forms
We have made enhancements to some of our forms and created an additional form to help make it easier for you to do business with Equitable Life®.
The first enhancement is an update to the ID Verification section to allow for Third Party ID Verification when a client doesn’t want to provide ID documents to an Advisor. They are now given additional options to either use the Alternative Identification requirements, or consent to Equitable Life verifying their identity through a third party service provider. We’ve also clarified in the Advisor declaration that they can’t sign for their own policies as they aren’t able to validate their own ID.
The above changes have been made to the following forms:- 671OC – Ownership Change Form
- 1027 – Additional/Updated Customer Information
- 1616 – Application for Term Conversion
The second enhancement is an update to Business forms. We’ve created a new form, 2004 Signing Authorities Certificate, to help Businesses provide the Signing Authority information needed more easily! Forms 594 and 682ENT have been updated to point to the new Form 2004 and also have new “Ownership structure” requirements added in section 2.
View the below forms for details on these changes:- 2004 – Signing Authorities Certificate (NEW)
- 594 – Business Information Form
- 682ENT – Claimants’ Statement for Entities
® denotes a registered trademark of The Equitable Life Insurance Company of Canada.
-
Manage more details within Contract Delivery for New Business applications
We are excited to announce further enhancements to our eDelivery process to empower you, the advisor, the ability to manage client details more easily within Contract Delivery.
Effective January 15, 2022, advisors will need to create a Password within Contract Delivery when choosing “eDelivery” as the contract delivery method and provide the password to the client to use as their password:
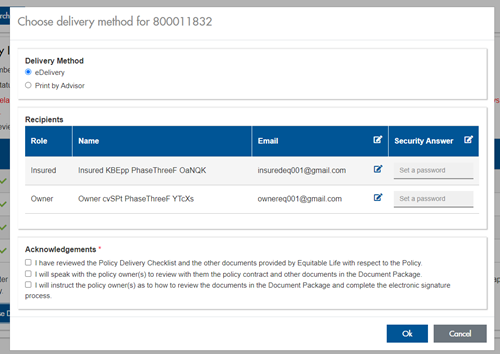
The Password must be between 4 and 100 alpha/numeric characters, and cannot be the Policy number. For multiple signers the password (and email address) must be unique per each signer.
Advisors can now edit and/or update an email address within Contract Delivery, in the event of a bounce back or email change, to keep the eDelivery process moving and avoid delays in processing time. If a lock out occurs, advisors can trigger a resend of the signing email once they add a new valid email address in Contract Delivery. Simply click the pencil icon beside the Email field to enter the valid email address:
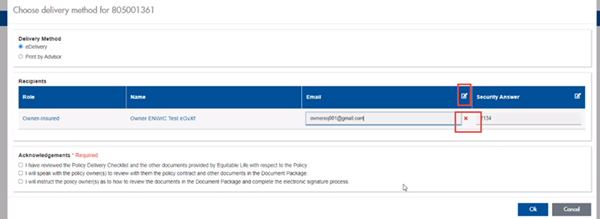
Another new feature- in the event a client has declined, the advisor will get an email from Equitable Life®. Click through to EquiNet® within the email to view the message within Contract Delivery that the client provided as the reason for decline under a new “Declined Details” section. This enables you to connect with the client to proceed with the sale by discussing the reasons for decline with them directly.
Also new for clients with this enhancement, policy owners of a policy created after January 15 will be able to see a PDF copy of their policy within client access. Note: this PDF copy is as the policy was originally issued.
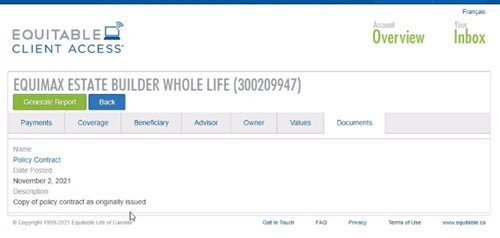
Resources: -
Equitable Life and Cloud DX
We have partnered with Cloud DX to provide remote monitoring for all our EquiLiving® Critical Illness Insurance eligible claimants.*
A Canadian first. Equitable Life’s Critical Illness eligible claimants, will now be supported beyond diagnosis and through treatment and recovery. Equitable Life is proud to announce that it has partnered with Canadian digital health innovator, Cloud DX, to provide a Virtual Monitoring Care service as part of its Critical Illness packages. We are pleased to offer this service on all new and existing EquiLiving coverages.
*Cloud DX is a non-contractual benefit and may be withdrawn or changed by Equitable Life® at any time. To be eligible for the Cloud DX offering, a claimant must be age 12 or older and have received payment on or after February 12, 2022 for a covered critical condition benefit under an individual critical illness insurance policy issued by Equitable Life. An early detection benefit payment does not qualify. Equitable Life pays for 6 months of Cloud DX subscription fees. If the claimant wishes to continue the Cloud DX service after 6 months, they will be responsible for the cost.
View our press release announcing Cloud DX and Equitable Life’s partnership, and watch our video featuring Donna Carbell, Senior Vice President, Individual Insurance.
