Site Search
466 results for enter now access MAKEMUR.COM Buying someones immediate bail Texas
-
Equitable Life Group Benefits Bulletin - October 2022
Introducing new Gender Affirmation Coverage for group benefits plans
Providing an inclusive benefits plan can play a critical role in fostering a workplace culture that welcomes diversity and helps employees thrive. While most provinces cover the cost of gender-affirming surgery, each person has unique needs. Some may require procedures that are not publicly covered.
That’s why we’re pleased to introduce a new coverage option for gender affirmation surgical procedures that are not covered by provincial health plans. Gender Affirmation Coverage helps plan sponsors to close the gap where provincial health coverage ends.Coverage details and eligibility
Gender Affirmation Coverage can be added to any Equitable Life plan with an in-force Extended Health Care plan. It provides coverage for gender-affirming procedures that are not covered by provincial health plans. This might include tracheal (Adam’s apple) shaving and voice surgery. It will also cover some additional procedures to further align the plan member’s features to the transitioned gender, such as facial bone reduction and cheek augmentation. This makes a wider variety of gender-affirming surgeries accessible to plan members and helps minimize their out-of-pocket costs.
Plan members are eligible for coverage with a diagnosis of gender dysphoria from a qualified health care professional.Offering a more inclusive benefits plan
The coverage provides one more way for your clients to offer more inclusive coverage and to offer holistic support to their plan members undergoing a gender transition. We have developed this coverage as a complement to our existing coverage options, including Health Care Spending Accounts (HCSAs), Taxable Spending Accounts (TSAs), Extended Health Care and drug coverage, and Employee and Family Assistance Programs, all of which can provide support to plan members undergoing gender affirmation.
We regularly review our products to ensure that they’re meeting your clients’ needs, and we’re committed to offering products that support diversity, equity and inclusion.
We also continue to review our forms, documents and processes to make them more inclusive. This includes reviewing our online plan member enrolment (OPME) tool to allow for more flexibility with the way plan members identify their gender.Gender affirmation and mental well-being
Gender affirmation procedures can lead to improved mental health outcomes for those with gender dysphoria, as most report an improvement in their quality of life following the procedures. Gender dysphoria may occur when a person’s assigned sex at birth does not match their identity, and people experiencing gender dysphoria typically report psychological and emotional distress, including symptoms of depression or anxiety. By offering coverage where provincial health coverage ends, your clients can support plan members as they seek procedures that align their body presentation with their self-identified gender.
Advantages at a glance
Advantages for plan members include:- Reimbursement for some procedures and expenses, leading to fewer out-of-pocket costs
- May experience improved mental health outcomes after surgery
- A benefits plan that promotes a culture of diversity, equity and inclusion, which may build employee loyalty
- Support for plan member mental health to help those with gender dysphoria thrive
The Benefits Canada 2022 Health Care Survey results are in!
Equitable Life is proud to be a Platinum sponsor for The Benefits Canada 2022 Health Care Survey, Canada’s leading survey on workplace benefits plans. This year’s survey report highlights many fascinating insights across a wide variety of benefits topics, including:- A focus on mental health for both plan sponsors and plan members
- The repercussions of the "shadow" pandemic due to health care delays
- Trends in plan members' overall perceptions of their health benefits plans
- The types of benefits getting more attention from plan members
- The role of remote work in plan member satisfaction
We’re committed to helping you and your clients navigate the evolving landscape of employee benefits in Canada by contributing to this vibrant industry community. To read the full report, visit Benefits Canada.
HCSA and TSA manual allocation reminder
If your clients’ Health Care Spending Account (HCSA) and/or Taxable Spending Account (TSA) have manual allocations, they need to allocate these amounts to plan members each year. Clients should review their plan members’ profiles on EquitableHealth.ca to ensure they have received their allocation(s) for the current benefit year. Your clients may also order HCSA and TSA forfeiture reports on EquitableHealth.ca.
If your clients have Plan Administrator update access on EquitableHealth.ca, they can update these amounts online by doing the following:- Select View certificate
- Select Health Care Spending Account or Taxable Spending Account
- Select Update Allocation in Task Center
- Enter amount in Revised Allocation Amount
- Override Reason – Plan Administrator Request
- Select Save
- Select Reports
- Select New
- Select Next
- Select HCSA or TSA Totals by Plan Member
- Select Next
- Enter end date of 12/31/2022
- Select Next
- Select Finish
- View Report
-
Easier group enrolment and more group benefits updates
Make enrolment easier for your clients with online plan member enrolment (OPME)
Enrolling new plan members can be overwhelming – for both you, your clients and their employees. It’s time-consuming to manually load new members and challenging to ensure they complete the necessary paperwork before the enrolment deadline.
Our Online Plan Member Enrolment (OPME) tool is available at no extra cost for all your Equitable Life clients and offers a more secure and efficient alternative to traditional paper enrolment. Using their computer or mobile device, employees can enrol in their benefits plan in just minutes.
The user-friendly tool allows plan members to easily enter all their enrolment information, including:- Dependent details
- Banking information for direct deposit of claim payments
- Details for coordination of benefits
- Beneficiary designation
The days of chasing plan members for their paper enrolment forms are gone. Once plan administrators enter a few employee details, our system automatically sends an email to each plan member, inviting them to enrol in their benefits program. And there will be no need for your clients to send reminders or follow up with employees about their benefits enrolment. It’s all done automatically.Support with using OPME
To learn more about the benefits of using OPME, check out our Online Plan Member Enrolment Flyer. We also encourage you to share more information with your clients: We also have helpful reference guides for plan members, to help them use the tool:- Online Plan Member Enrolment Quick Reference Guide
- myFlex Online Plan Member Enrolment Quick Reference Guide
Help your clients spend less time administering group benefits. Contact your Group Account Executive or myFlex Sales Manager to learn more about our online plan member enrolment.
Coming soon: A survey to help us serve your clients better*
We are committed to providing your clients and their plan members with industry-leading service. We’ve introduced several enhancements over the past year to make it easier to do business with us. And we’re continually looking for ways to improve.
This month, we will conduct a survey of your clients to help us understand how we can better serve them. Plan administrators will receive an email with a link to the survey, which will take between five and 10 minutes to complete.
Please encourage your clients to participate. Their feedback will be confidential, and their responses will help us improve our service and ensure we’re meeting their expectations. We will also allow them to provide their name so that we can follow up with them to address any concerns they’ve identified.
We know your clients’ time is valuable. So, each plan administrator who completes the survey will be entered into a random draw for a chance to win one of 3 prepaid gift cards for $200.
Improved mental assessment features for FeelingBetterNow®*
Mensante has enhanced its FeelingBetterNow® online platform to make it easier for plan members to assess the state of their mental health and talk to their health care provider about treatment options. FeelingBetterNow is part of our Equitable HealthConnector suite of wellness solutions and is available for an additional cost. It can help plan members easily identify if they are at risk for a number of common mental health issues, including depression, anxiety and substance abuse.Upgrades to the platform include:
- New features to help plan members better gauge their progress in the assessment.
- A printable Action Plan that plan members can share with their health care provider to initiate conversations about managing their mental health challenges.
- A new “follow-up” module to help plan members assess the care they’ve received from their health care provider and identify care gaps.
- An Assessment Outcome Page, which allows plan members to view their diagnostic risks across mental health disorders for a more holistic picture of their health.
Over-age dependants losing coverage?*
Your clients’ plan members may have dependants approaching the maximum age for eligibility under their group benefits plan. If so, members should be aware of their options for dependant coverage.Coverage for full-time students and dependants with disabilities
The dependants of your clients’ plan members may be eligible to continue their coverage under the current plan if:- The dependant is attending a post-secondary school full-time; or
- The dependant is disabled.
Coverage2go for over-age dependants
Dependants who aren’t eligible for continued coverage under the plan can apply for Coverage2go®, a month-to-month health and dental plan for individuals losing their group coverage.**
Coverage2go is affordable, reliable and allows the over-age dependants to choose the level of coverage and protection that suits their personal situation. With no medical questions required as long as they apply within 60 days of losing their coverage, your clients’ plan members can ensure that their over-age dependants have the coverage they need.
Plan members can receive a quote within minutes. Please direct your clients to Coverage2go on Equitable.ca to learn more.
**Quebec residents are not eligible for Coverage2go.Forfeiture reports for HCSAs and TSAs on EquitableHealth.ca*
As a reminder, your clients can access forfeiture reports for their Health Care Spending Account (HCSA) and Taxable Spending Account (TSA) usage on EquitableHealth.ca.HCSA summary by plan member
HCSA summary reports provide an overview of each plan member’s account activity and balances. These reports include the total amounts allocated, the amount claimed to date, the net balance, and the amount of funds that will be forfeited based on claims paid to date. Please note that plan members’ claim submissions will remain confidential and will not be viewable by the employer on this summary.
Your clients can provide each plan member with their HCSA summary, if they wish.HCSA account forfeiture by plan member
HCSA forfeiture reports detail the amount that each member will forfeit if they do not use it. The amount is based on claims that have been paid to date within the benefit year period.HCSA account totals by plan member
Your clients may wish to access the HCSA account totals reports, which reflect the information in each plan member’s HCSA summary report. For terminated employees, the Funds Available field will display as zero, regardless of the balance in the account when terminated.
At least three months before the end of the benefits period, your clients should remind their members to use their allocated HCSA and TSA amounts.
If your clients need help accessing these reports, they can reach out to their Regional Office Service team for assistance.
* Indicates content that will be shared with your clients.
-
Equitable Life Group Benefits Bulletin - September 2022
Homewood Health launches Sentio, an upgraded iCBT platform
Equitable Life’s mental health partner, Homewood Health, has launched Sentio, an upgraded platform for Internet-based cognitive behavioural therapy (iCBT). This self-directed platform is now available to all Equitable Life clients, and it replaces Homewood’s previous iCBT platform, i-Volve.
Sentio Self-Directed iCBT is a comprehensive digital cognitive behavioural therapy platform. Developed by Homewood’s mental health experts, it is an action-oriented solution for plan members, giving them practical resources and activities to help with their depression, anxiety and overall mental health challenges.
Available as a standalone app, on mobile, tablet and desktop, Sentio contains over 20 unique treatment goals for issues like stress management, improving sleep, managing depressive thoughts, and coping with panic. Users can work through treatment goals in any order, at their own pace. It also includes tools and resources to help plan members build skills and change their thought patterns.Sentio iCBT benefits
Sentio integrates seamlessly with Homewood Pathfinder so that users can easily locate and take advantage of the iCBT activities available. Sentio also includes a number of unique features:- More interactive features and activities to help plan members build valuable mental health skills
- Integrated symptom measurement and progress tracking
- Interactive multimedia learning and cognitive exercises to enhance learning
- Progress, learnings, and exercises that have been accessed are available to be re-accessed for 12 months
Please contact your Group Account Executive or myFlex Sales Manager if you have any questions.
Streamlining disability claims with Opifiny
Equitable Life is partnering with Opifiny to provide a quicker and more seamless disability claims experience.
Opifiny is an online platform that streamlines the disability claims process for consulting physicians, benefits plan sponsors, and disability plan members. Equitable Life will be using Opifiny for ongoing disability claims management, modernizing the process of gathering medical assessments and information.
Disability claims frequently involve several instances of correspondence between Equitable Life and the plan member’s medical team. By using the secure platform, health care professionals can access, respond to and process medical insurance requests easily from any device. They can typically complete administrative tasks associated with disability claims in a quarter of the time. The platform is secure and protects the privacy of their patients’ confidential information.
By digitizing and modernizing the claims management process for doctors, Equitable Life will have faster access to higher quality claims information. For some claims, using Opifiny may enable Equitable Life to help plan members safely return to work sooner.
Reminder: Obtaining plan member signatures on all administration forms
Please remind your clients that plan members must sign all administration forms, including enrolment forms, benefits change forms, and beneficiary designation forms. Once completed, a plan administrator can keep the form or send it to us. We are not able to accept a beneficiary designation that has not been signed by the plan member. Having appropriately signed forms helps to ensure that any life insurance claims are paid to the intended recipients.
For your clients’ convenience, forms can be signed electronically using one of our approved vendors, which include DocuSign, BambooHR, Adobe Sign, and many more.
If you have questions about providing signed forms, please contact your Group Account Executive or myFlex Sales Manager.
Correction: Coverage for full-time students and dependents with disabilities
In our August edition of eNews, we provided incorrect information about benefits coverage options for over-age dependents. We indicated that over-age dependents who are full-time students may continue to be eligible under the plan member’s benefits plan if they are studying in their home province. However, attending a post-secondary institution in their home province is not a requirement for continued eligibility. Dependents who are full-time students may continue to be eligible for coverage regardless of where in Canada they are attending post-secondary education.
If your clients have any questions about extending coverage for over-age dependents that are full-time students, please notify them of this error.
We apologize for any inconvenience or confusion this may have caused.
- [pdf] Do you know Dakari and Ash
-
August 2019 Advisor eNews
Coming soon:
Tech updates for plan members
Technology doesn’t stand still, and neither does your clients' businesses. That’s why we continually invest in technology to make things easier for your clients and their employees.
Faster claims processing on Equitable EZClaim® Mobile
Equitable Life now provides real-time processing of massage therapy, physiotherapy and chiropractor claims submitted via the EZClaim Mobile app.
That means plan members are able to find out the status of their claim almost instantaneously. And, for approved claims, they will receive payment even sooner - often in as little as 24 hours.
In order to allow for instantaneous processing and faster payment, plan members will be prompted to enter some additional information including the practitioner’s name, the date of the expense, and the type and amount of the expense, when submitting their claims for these services.
Equitable Life plan members can submit all types of health and dental claims via EZClaim Mobile, including co-ordination of benefits and Health Care Spending Account claims. Currently, 43% of all claims are submitted through the user-friendly app.
AS part of our ongoing efforts to improve the mobile claims experience for plan members, we've also added biometric login functionality to allow plan members to sign in to the app using their face or fingerprint. And we've redesigned our landing page on the mobile app to make it easier for plan members to navigate the various features of the app.
We will be announcing this enhancement to plan members on EquitableHealth.ca
Introducing InpatProtect:
Health coverage for employees who are new to Canada
For a new employee starting to work in Canada, looking after basic health needs can be difficult.
There’s a waiting period for provincial health coverage, and group benefits plans don’t cover the physician, hospital or emergency services that they or their eligible dependents may need during their initial months in the country. They could end up incurring significant unexpected health expenses.
That’s why Equitable Life has launched InpatProtectTM. InpatProtect provides temporary coverage to look after the basic health needs of employees and their eligible dependents during their transition to Canada. Your clients can recruit from outside the country knowing that their employees will have some protection in the event of a medical need, including an emergency.
For up to 90 days, InpatProtect will cover employees and their eligible dependents for basic services that would normally be reimbursed under provincial health plans, such as:
- Physician services
- Prescriptions for medications
- Diagnosis and treatment for illness or injury
- Hospital services
- In-patient services
- Drugs prescribed and delivered as an inpatient in-hospital
- Out-patient services
- Emergency services
- Ambulance services
- Emergency dental services
Contact your Group Marketing Manager or myFlex Sales Manager for more information about this new product from Equitable Life.
De-listed service providers
As part of our ongoing initiative to have Group Benefits plans only reimburse eligible claims, we conduct reviews of the billing and administrative practices of service providers, including clinics, facilities and medical suppliers.
As a result of these reviews we may de-list certain providers. We will no longer accept, or process claims for services and/or supplies obtained from those providers. The plan member can still choose to obtain services or supplies from these providers, but Equitable Life will not provide reimbursement for the claims.
Review Equitable Life’s de-listed service providers
The delisted service provider list is also posted on EquitableHealth.ca for plan members to review to determine if their claim(s) are eligible for reimbursement under their Group Benefits plan.
For more information about protecting group benefits plans from abuse, check out our articles.
1 Based on Equitable Life health and dental claims submitted between January 2019 – March 2019
Google Home and Google Assistant are registered trademarks of Google LLC.
® denotes a trademark of The Equitable Life Insurance Company of Canada unless otherwise indicated. - Physician services
-
Announcing Equitable Life's National Biosimilar Program
Beginning March 1, 2024, we are expanding our biosimilar switch program nationally** to protect all our clients and to make our coverage consistent across Canada.
Our national biosimilar initiative will simplify drug plan coverage, replacing our provincial programs with one program across the country.
Why now?
Over the past few years, most provinces have introduced policies to delist some originator biologic drugs. They require most patients to switch to biosimilar versions of those drugs to be eligible for coverage under their public drug plans. Soon, it is expected that all provincial drug plans will cover only biosimilars.
In response, we have implemented biosimilar switch initiatives in BC, Alberta, Saskatchewan, Ontario, Quebec, New Brunswick and Nova Scotia to align with these provincial changes. Our initiatives are designed to protect our clients from additional drug costs that may result from these government policies while providing access to equally safe and effective lower cost biosimilars.
How will this affect clients’ drug plans?
Because we have already introduced biosimilar switch initiatives in most provinces, the impact of this change will be minimal. It will primarily affect plan members in provinces or territories where we haven’t already required the switch to biosimilars, and plan members who are taking biosimilars that were not originally included in the switch initiative for their province.
Regardless of where they live, plan members across Canada will no longer be eligible for most originator biologic drugs if they have a condition for which Health Canada has approved a lower cost biosimilar version of the drug. Plan members already taking the originator biologic will be required to switch to a biosimilar version of the drug to maintain coverage under their Equitable plan. We will support their transition with education, personalized communication, and resources.
Will this change affect clients' rates?
Any cost savings associated with the change will be factored in at renewal.
Biologics are drugs that are engineered using living organisms like yeast and bacteria. The first version of a biologic developed is known as the “originator” biologic. Biosimilars are highly similar to the drugs they are based on, and Health Canada considers them to be equally safe and effective for approved conditions.
What is the difference between biologics and biosimilars?
Advance notice
We will be communicating with affected claimants in early December to allow them ample time to change their prescription and avoid any interruptions in their treatment or their coverage.
If you have any questions about this change, please contact your Group Account Executive or myFlex Account Executive.
**Excludes plan members in Quebec who participate in a separate provincial program. -
Celebrating our most popular Pivotal Select funds
In August 2022, Equitable® launched 12 new segregated funds in Pivotal Select’s Investment Class (75/75). We wanted to bring some new innovative solutions to the product, including six sustainable investment funds. To say the launch of these funds was successful would be an understatement.
The funds are quickly becoming some of the most popular funds in Pivotal Select™, and their performance in 2023 was impressive. Equitable wants to celebrate these funds and encourage clients to consider them for their portfolios.
As of February 29, 2024, nine out of the 12 funds received a 1st quartile ranking for their 1-year return and two more were 2nd quartile. The table below shows the new funds that ranked in the top two quartiles for their 1-year returns.
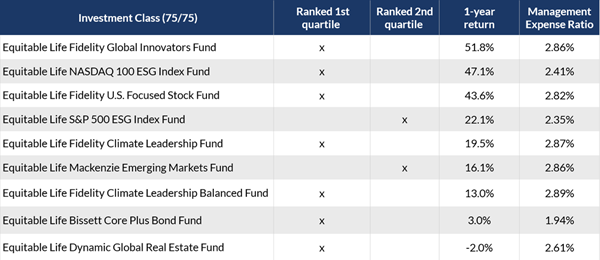
Access additional fund performance information
If you haven’t looked at these funds yet, now is the time. Speak to clients about their investment options and see if these funds fit within their investment portfolio.
Talk to your Director, Investment Sales today for more information.Disclaimer
Any amount that is allocated to a segregated fund is invested at the risk of the contractholder and may increase or decrease in value. Segregated fund values change frequently, and past performance does not guarantee future results. Investors do not purchase an interest in underlying securities or funds, but rather, an individual variable insurance contract issued by The Equitable Life Insurance Company of Canada. There are risks involved with investing in segregated funds. Please read the Contract and Information Folder before investing for a description of risks relevant to each segregated fund and for a complete description of product features and guarantees. Copies of the Contract and Information Folder are available on equitable.ca.
Management Expense Ratios (MERs) are based on figures as of February 29, 2024, and are unaudited. MERs may vary at any time. The MER is the combination of the management fee, insurance fee, operating expenses, HST, and any other applicable non-income tax for the fund and for the underlying fund. For clients with larger contract values, a Management Fee Reduction may be available through the Preferred Pricing Program. For details, please see the Pivotal Select Contract and Information Folder.
® and TM denote trademarks of The Equitable Life Insurance Company of Canada.
Posted April 18, 2024
-
Enhancing the Transfer Process: Equitable's New Signature Guarantee Service
Equitable® is making transfers even easier with EZcomplete®.
This enhancement will help advisors and clients by reducing the number of rejections from other institutions that need a signature guarantee. Reducing transfer rejections means less time and effort for advisors, and faster transfers from other institutions.
Signature Guarantees
Equitable will now offer signature guarantees on most transfers requested through EZcomplete.
When is a signature guarantee not available?
• For entity owned accounts
• If a Power of Attorney is signing on behalf of an owner
• If the transferring account has an irrevocable beneficiary
Watch the quick Identity Check with Persona video or read through instructions below.
To offer a signature guarantee, Equitable first needs to check the identity of all owners using Persona, a third-party service provider.
The advisor starts by selecting a signature guarantee in EZcomplete. An email link is sent to all proposed owners.
Clients can click the link within the email to Persona's verification process.
They will be prompted to take a picture of their photo ID and a selfie, turning their head slightly left and right by following the prompts.
Their identity can then be confirmed in seconds.
Sending Transfer Forms:
• If all owners' identities are verified, Equitable will send the transfer form with a signature guarantee stamp and the e-signature audit log to the transferring institution.
• If ID verification fails, clients will be prompted to try up to three times. If still unsuccessful, the transfer form and e-signature audit log is sent to the transferring institution without the signature guarantee stamp.
Handling Issues:
• Advisors’ obligations to verify ID is not affected by this process; ID verification is still required.
• If the client times out or loses the email to access Persona, the advisor can resend the link.
• If the client’s name or email changes after ID verification, the advisor will need to redo the ID verification with the updated information to get a signature guarantee.
This update strives to make processes smoother and more efficient for everyone. Just another reason to do business with Equitable. When we work together, success is mutual.
For more information or assistance, please contact your Director, Investment Sales.
Date published: May 7, 2025 - Administration Reference Guide for Individual Wealth
-
Have you heard about Equitable Client Access?
Equitable Client Access® allows clients to self-serve on some of the more popular requests. Thousands of clients have already signed up for Equitable Client Access and are enjoying the benefits of accessing their secure information 24/7.
• Does your client need to change or stop existing Pre-Authorized payment (PAD)? Equitable Client Access can do that.
• Does your client need to change a withdrawal date for a PAD? Equitable Client Access can do that too.
• Address or banking information changes? Equitable Client Access has your clients covered.
• Does your client need to change her beneficiary from Aunt Flora to Uncle Ned? Equitable Client Access can even do that.
Equitable Client Access is a secure online client site that connects clients with policy information, right at their fingertips. In addition to the self-serve features, Equitable Client Access can also provide:
• Insurance coverage and guarantees
• Investment allocation, performance and market values
• Transaction history
• Statements and letters
• Advisor contact information, along with so much more.
If your clients have not signed up for Equitable Client Access, direct them to client.equitable.ca - it only takes a few minutes to set up an account, and connects your clients with their policy information online – anytime!
Have a question about Equitable Client Access? Want to tell your client how to go paperless? Check out our updated FAQ or contact your Regional Investment Sales Manager today.
