Site Search
633 results for access link PROBLEMGO.com how much to make customs overlook a violation
-
THREE new ways to help make your Savings & Retirement business run smoother
As of August 20, 2022, EZcomplete® will include several new features that allow applications to be completed faster and easier:
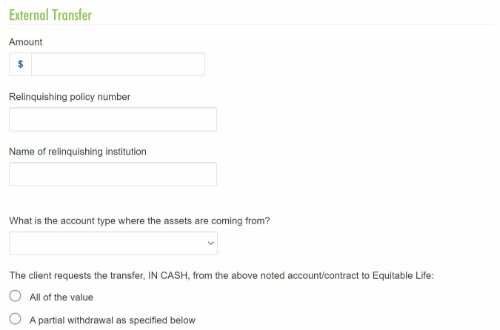
1. Prefilled Fund Transfer Form
The transfer form will be generated with the information from EZcomplete and included in the EZcomplete signing package, saving you time.
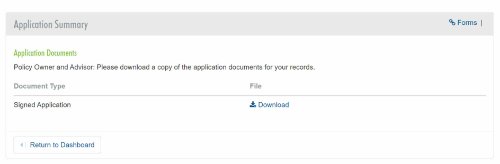
2. Client eSignature Audit History and Document Download
If you choose the e-signature option for the client, you’ll be able to download a copy of the e-signed transfer forms and the signature audit history.
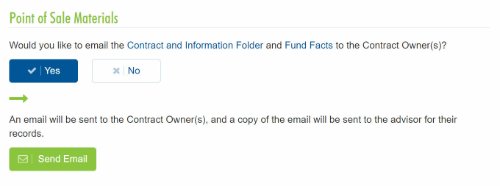
3. Email the Client Contract Info and Fund Facts Before Signing
You'll now be able to email Point of Sale materials (Contract & Info Folder and Fund Facts) to clients before they provide their e-signature.
Log in to EZcomplete today!
Speak to your Regional Investment Sales Manager to learn more!
-
Mental health support for all plan members
As the COVID-19 pandemic continues, many Canadians are dealing with increased stress and anxiety. Now, more than ever, plan members need easy to access resources to help them cope with these uncertain times.
Through our partnership with Homewood Health®, the Canadian leader in mental health and addiction services, all of our clients and their plan members have access to tools designed to provide guidance and support, including i-Volve, Homewood’s Online Cognitive Behavioural Therapy tool.
Proven therapy, at your own pace
Included with Homewood Online resources in every Equitable Life® plan, i-Volve can help plan members identify, challenge and overcome anxious thoughts, behaviours and emotions. It encourages incremental changes in behaviour and is proven to be an effective therapeutic approach for dealing with mild to moderate anxiety or depression. Plan members work at their own pace through a series of web-based exercises, ultimately helping to change the ways in which they think, feel and react in various situations.
Free for all Equitable Life plan members
All Equitable Life clients and their plan members have access to i-Volve. It’s available 24 hours a day, seven days a week, wherever you choose to access it.
Contact your Group Account Executive or myFlex Sales Manager to learn more about Homewood Health and i-Volve Online CBT. - [pdf] A better group benefits experience
-
January 2023 eNews
Responding to Saskatchewan’s biosimilar switch initiative*
We are changing coverage for some biologic drugs in Saskatchewan in response to the province’s biosimilar initiative. These changes will help protect your clients’ plans from additional drug costs that may result from this new government policy while providing access to equally safe and effective lower-cost biosimilars.
Saskatchewan’s provincial biosimilar initiative
Announced in October 2022, the Saskatchewan Biosimilars Initiative ends coverage of ten biologic drugs beginning on April 30, 2023.
Patients in the province who are using these drugs will be required to switch to biosimilar versions of these drugs by April 30, 2023, in order to maintain their Saskatchewan Drug Plan coverage.
Equitable Life’s response
To ensure this provincial change doesn’t result in your clients’ plans paying additional and avoidable drug costs, we are changing coverage in Saskatchewan for most biologic drugs included in the provincial initiative.
Beginning April 30, 2023, plan members in the province will no longer be eligible for most originator biologic drugs if they have a condition for which Health Canada has approved a lower cost biosimilar version of the drug.** These plan members will be required to switch to a biosimilar version of the drug to maintain coverage under their Equitable Life plan.
Communicating this change to plan members
We will inform any affected plan members in early February of the need to switch their medications so that they have ample time to change their prescriptions and avoid any interruptions in treatment or coverage.
What is the difference between biologics and biosimilars?
Biologics are drugs that are engineered using living organisms like yeast and bacteria. The first version of a biologic developed is known as the “originator” biologic. Biosimilars are highly similar to the drugs they are based on and Health Canada considers them to be equally safe and effective for approved conditions.
Questions?
If you have any questions about this change, please contact your Group Account Executive or myFlex Sales Manager.
**The list of affected drugs is dynamic and will change as Saskatchewan includes more biologic drugs in its biosimilar initiative, as new biosimilars come onto the market, and as we make changes in drug eligibility.
Ontario announces 2023 biosimilar switch program*
The government of Ontario recently announced the launch of a biosimilar initiative to switch patients from eight originator biologic drugs to biosimilar versions of the drugs.
Patients in Ontario using affected originator biologic drugs will have until December 29, 2023 to switch to a biosimilar version of their medications in order to maintain coverage under the province’s public drug plans.
We are actively monitoring and investigating the impact of this new policy on private drug plans in Ontario. We plan to implement changes to coverage of biologic drugs in the province in 2023 to help prevent this change from resulting in additional costs for our clients’ drug plans. We will provide more details in the coming months.
If you have any questions, please contact your Group Account Executive or myFlex Sales Manager.
Dental fee guide updates*
Each year, Provincial and Territorial Dental Associations publish fee guides. Equitable Life® uses these guides to help determine the reimbursement limits for dental procedures. For your reference, below is the list of the average dental fee increases for general practitioners that will be used by Equitable Life for 2023.***Dental fee guide increases over 2022***

***Data for all provinces and territories was not available at the time of publication. This chart will be updated on EquitableHealth.ca as more information becomes available.
Equitable Life ranks high with Canadian group advisors*
Equitable Life ranked second nationally and first in Ontario among major insurers in a recent survey of Canadian group benefits advisors.
NMG Consulting, a leading global consulting firm, conducted in-depth interviews with 130 leading group consultants, brokers and third-party administrators across the country between May and August 2022 for its annual Canadian Group Benefits Study. Based on these interviews, NMG ranked group insurers in six categories, ranging from operational management to technology.
Nationally, Equitable Life ranked either first or second in four of the six main categories:

Advisors in Ontario, in particular, scored Equitable Life very favourably. We ranked #1 overall in the province, finishing first in four of the six overall categories, including: Relationship Management, Operational Management, Underwriting and Claims Management and Technology.
“The fact that advisors regard us so highly in so many categories is a testament to our mutual status and our ability to focus exclusively on our clients and advisors,” said Marc Avaria, Senior Vice President of Group. “We are truly working together to build strong, enduring and aligned partnerships.”
“While we are happy with these results, we won’t rest on our laurels,” added Avaria. “We will continue to dedicate ourselves to providing our clients and advisors with a better benefits experience.”
Here are more of the highlights from this year’s results:
Nationally, we ranked first in all 10 subcategories in Operational Management, including:- Overall service to intermediaries,
- Overall service to plan sponsors,
- New quote process,
- Plan implementation,
- Renewal process,
- Information shared at renewal,
- Accuracy and timeliness of reporting and billing,
- Administration quality and responsiveness,
- Taking ownership and
- Management information quality and availability.
- Company relationship management,
- Ease of doing business,
- Account executive capability,
- Market knowledge,
- Visit/call quality,
- Effective coordination and
- Advice.
- Fairness and timeliness of disability claims (1st)
- Fairness and timeliness of health claims (2nd)
- Fraud management (2nd)
- Competitiveness of pooling charges (2nd)
- Group underwriting flexibility (3rd)
- Health and dental TLR competitiveness (3rd)
- Overall technology – Intermediary (2nd)
- Member experience (2nd)
-
February 2023 eNews
Responding to Nova Scotia’s biosimilar switch initiative
We are changing coverage for some biologic drugs in Nova Scotia in response to the province’s biosimilar initiative. These changes will help protect your clients’ plans from additional drug costs that may result from this new government policy while providing access to equally safe and effective lower-cost biosimilars.Nova Scotia’s provincial biosimilar initiative
Announced in February 2022, the Nova Scotia Biosimilar Initiative ends coverage of seven biologic drugs for residents enrolled in Pharmacare programs.
Pharmacare patients in the province using these drugs will be required to switch to biosimilar versions of these drugs by February 3, 2023, in order to maintain their Nova Scotia Pharmacare coverage.Equitable Life’s response
To ensure this provincial change doesn’t result in your clients’ plans paying additional and avoidable drug costs, we are changing coverage in Nova Scotia for most biologic drugs included in the provincial initiative.
Beginning June 1, 2023, plan members in the province will no longer be eligible for most originator biologic drugs if they have a condition for which Health Canada has approved a lower cost biosimilar version of the drug.** These plan members will be required to switch to a biosimilar version of the drug to maintain coverage under their Equitable Life plan.Can my client maintain coverage of these biologic drugs?
Traditional groups who wish to opt out of this change and maintain coverage of these originator biologics for Nova Scotia plan members can submit a policy amendment. Amendments must be submitted no later than April 1, 2023. Advisors with myFlex Benefits clients who wish to maintain coverage of these originator biologics for Nova Scotia plan members should speak to their myFlex Sales Manager to confirm their eligibility to opt out of this change.
Groups that choose to maintain coverage of these originator biologics for existing claimants will also maintain coverage for any originator biologics that we subsequently add to our Nova Scotia biosimilar initiative.Will this change impact my clients’ rates?
The rate impact of this change in coverage will be relatively insignificant. Any cost savings associated with the change will be factored in at renewal.
If plan sponsors opt out of these changes and maintain coverage for the originator biologics, it may result in a rate increase. Any rate adjustment will be applied at renewal.Communicating this change to plan members
We will inform any affected plan members in April of the need to switch their medications so that they have ample time to change their prescriptions and avoid any interruptions in treatment or coverage.What is the difference between biologics and biosimilars?
Biologics are drugs that are engineered using living organisms like yeast and bacteria. The first version of a biologic developed is known as the “originator” biologic. Biosimilars are highly similar to the drugs they are based on and Health Canada considers them to be equally safe and effective for approved conditions.Questions?
If you have any questions about this change, please contact your Group Account Executive or myFlex Sales Manager.
**The list of affected drugs is dynamic and will change as Nova Scotia includes more biologic drugs in its biosimilar initiative, as new biosimilars come onto the market, and as we make changes in drug eligibility.
Changes to New Brunswick drug interchangeability rules
We are introducing changes to help ensure that your clients with voluntary or mandatory generic pricing for their drug plans will benefit more from the cost savings of these two features, regardless of the province where the drugs are dispensed.
Currently, when determining whether a lower-cost alternative is available for a brand-name drug, most insurers only consider drugs that the provincial drug plan identifies as interchangeable.
However, the public drug plan in New Brunswick does not identify a drug as interchangeable if the drug is not listed on its formulary – even if Health Canada has deemed the drug interchangeable.
As a result, plans with mandatory or voluntary generic pricing have continued to reimburse some drugs in New Brunswick based on the cost of the brand-name drug, even if a lower-cost generic alternative is available.
Effective March 20, 2023, if your clients have drug plans with mandatory or voluntary generic pricing, we will adjudicate any drug claims in New Brunswick using the lowest cost alternative that Health Canada approves as bioequivalent. This will occur even if the public drug plan has not identified the drug as interchangeable.
To benefit from this more robust drug plan control, plan sponsors must have mandatory or voluntary generic pricing in place.
For more information about this change or about implementing mandatory or voluntary generic pricing for your clients, please contact your Group Account Executive or myFlex Sales Manager.
New template: plan members eligible for additional coverage
Often, based on salary, some plan members may become eligible to apply for extra Life, Accidental Death & Dismemberment (AD&D), Short Term Disability or Long Term Disability coverage. If this occurs, your clients receive a notification from Group Benefits Administration. We have now developed a template that your clients can provide to applicable plan members if they become eligible for extra coverage. The template makes it simpler for your clients to pass on these details to their plan members efficiently.
The new template is available for download under the Quick Links section of EquitableHealth.ca. It is a fillable PDF form that your clients can complete and provide to their plan members when necessary. The document is called Over the Non-Evidence Limit for Plan Members Notification.
If you have any questions about the template, please contact your Group Account Executive or myFlex Sales Manager. - [pdf] TFSA Third Party Contribution
- Brandes
- [pdf] Daily/Guaranteed Interest Account Client Brochure
- [pdf] Health Care Spending Account - Plan members
- Pre-Authorized Payments
