Site Search
378 results for pre-authorized debit plan
-
Insights from a pandemic: Long-term COVID-19 drug risks
For the remainder of 2020 and beyond, COVID-19 will continue to add to the existing pressures driving up drug costs. Examples of contributing factors include:
- Claims for acute drugs will likely increase as elective surgeries resume and plan members address non-emergency health issues that were left unattended during COVID-19.
- Plan members whose employers are facing financial strain due to COVID-19 may stock up on their prescriptions in anticipation of losing their job and/or their benefits.
- An ongoing increase in the prevalence and severity of mental health issues and chronic conditions. In May and June, we saw a dramatic increase in the number of claimants for depression, ulcers, blood pressure and diabetes, and depression was associated with 1 in 5 claimants.
All trends thus far suggest we can expect about a 10% increase in average paid amounts per certificate in 2020 compared with 2019. But the impact won’t be the same for all groups. There will be significant variations, particularly for smaller groups, and some may see much larger cost increases.
Unknown COVID-19-related risks
Another risk exposure may come from the costs associated with drugs used to treat or prevent COVID-19. There are currently numerous vaccines in development, and more than 300 clinical trials are underway for both new and existing drugs to determine their effectiveness in treating the virus.
The cost of any vaccine or whether government or private plans will pay for it is unknown. Regardless, there will likely be other drugs indicated for the treatment or prevention of COVID-19 that private plans will be expected to cover. The cost of this impact for private payers is unknown, but potentially high.
Another unknown is what will happen with dispensing fees. While most provinces have lifted their 30-day prescription refill limits, it remains to be seen whether pharmacies will resume dispensing 60- and 90-day refills at pre-COVID levels for private plans. If not, this would mean the dispensing fees will continue to drive up drug costs.
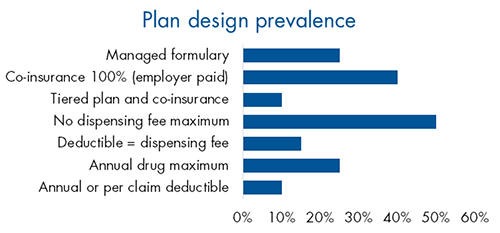
Advisor opportunity
Despite the increase in drug plan risk in recent years, little has changed in plan design trends. Very few plan sponsors have adopted managed plans or other plan design options that could help manage risk.
This presents an opportunity for advisors to educate their clients about the risks their drug plan may be exposed to and the options available to manage that risk.
A practical starting point for those conversations is our Drug Plan Design Tool. With two simple questions, it can help confirm your client’s objectives and identify some best-fit solutions for their plan. Ask your Group Account Executive or myFlex Sales Manager for a copy of the tool.
-
Equitable Life Coronavirus Update – March 13, 2020
As the coronavirus (COVID-19) continues to spread, it’s important that you, your clients and their plan members have the most up-to-date information. We are providing timely updates on any developments that impact your clients and their plan members or their benefits coverage.
Please share this information with your clients. You can direct them to EquitableHealth.ca, where we have posted a version of these updates.
Coronavirus travel coverage*
For groups with Travel Assist coverage
The Public Health Agency of Canada has issued several Travel Health Notices advising Canadians to avoid travel to countries and regions where there have been outbreaks of coronavirus (COVID-19).
A good resource to help your clients and their plan members understand how the spread of the coronavirus may impact their travel plans is the Public Health Agency of Canada’s Coronavirus Travel Advice site. The levels of risk by country and region are regularly updated.
If your clients’ plan members cannot avoid travelling, Public Health recommends they take steps to prevent illness and seek medical attention if they become sick.
Where to find the latest information
The list and level of travel advisories can change at any time. Please check the Government of Canada’s Travel Advisor and Advisory page for the most current information.
If your clients’ plan members have coronavirus symptoms while travelling, please advise them to contact Travel Assist at the numbers listed below for assistance.
Advise plan members to call before they travel
If a plan member is travelling anywhere outside of the province or country and their benefits plan includes Travel Assist, plan administrators should advise them to make sure they’re prepared for a medical emergency by following these steps.
- Check the Government of Canada’s Travel Advisor and Advisory page. Note that it is important to click on the country to check whether any specific regions of that country have travel advisories.
- If they have questions, they should call Travel Assist before they travel for assistance and benefit information.
- Pack their Equitable Life benefits card and provincial health card.
- In a medical emergency, call the Travel Assist 24-Hour Hotline:
- Toll-free Canada/USA: 1.800.321/9998
- Global call collect: 519.742.3287
- Allianz Global Assistance ID #9089
Allianz Global Assistance administers Equitable Life’s Travel Assist benefits. Allianz has an international network of medical facilities, transportation providers, medical correspondents and multilingual administrative agents who aid with medical, legal and most travel-related emergencies 24-hours a day, seven days a week.
Early prescription refills and drug shortages*
In response to concerns about COVID-19 TELUS Health, our pharmacy benefits manager, has announced it is maintaining its standard rules for refills of medication. Plan members can refill their medications when at least two-thirds of the last dispensed supply has been used.
If plan members need more than the maximum supply allowed on their plan, they must pay out-of-pocket for the excess amount. They can then submit a claim to ask for an exception request.
TELUS is taking this position to help maintain access to medication for all patients. They continue to monitor the situation. We will provide an update if it changes.
Drug shortages
TELUS Health monitors for drug shortages and updates their system for any unavailable drugs. This helps to ensure accurate claims payment. If a referenced lowest-cost generic drug is unavailable, claims for drugs in the class will be paid at the next lowest-cost generic alternative available.
*Indicates content that will be shared with your clients
-
Equitable Life Group Benefits Bulletin - July 2021
In this issue:
- Fabien Jeudy takes over as President and CEO*
- Reminder: Equitable Life’s Guide to Accessing Virtual Healthcare*
- Mental health resources for plan members*
- Recall of Philips CPAP machines*
Fabien Jeudy takes over as President and CEO*
In March, we announced that Fabien Jeudy was appointed as Equitable Life’s next President and CEO. Jeudy officially took over on July 5th, succeeding Ronald Beettam, who is retiring after 16 years with the company.
Jeudy is a collaborative leader with more than 30 years of experience in the insurance industry, leading actuarial, finance, risk management, distribution, marketing teams and operational teams in the Life & Health Insurance, Wealth Management and Group Benefits markets in Canada, the US, and Asia.
Reminder: Equitable Life’s Guide to Accessing Virtual Healthcare*
The demand for virtual healthcare services has increased as the pandemic is driving more people to access their health care providers from home.
Thankfully, many virtual healthcare services are available for free to Canadians with provincial health care coverage. We have created a Guide to Accessing Virtual Healthcare for plan members to easily access a variety of virtual healthcare services. Our guide includes information and links to both free and paid virtual medical care options, including video appointments, health advice over the phone, emergency dental services, and more.
You can find the guide on our website. It’s also available on our plan member website at EquitableHealth.ca.Mental health resources for plan members*
Many Canadians have been experiencing increased levels of stress, anxiety, and depression since the beginning of the COVID-19 pandemic. Through our partnership with Homewood Health®, all of our clients and their plan members have access to a number of health and wellness resources designed to provide guidance and support.
Homewood’s Online Cognitive Behavioural Therapy tool, i-Volve, can help plan members identify, challenge and overcome anxious thoughts, behaviours and emotions. Learn more about Online CBT or access i-Volve at Homeweb.ca/Equitable.
As well, Homewood has a number of resources available to help support plan members dealing with increased anxiety during these uncertain times:- Quelling COVID-19 Anxiety
- Managing stress and anxiety
- How to speak to children
- How to stay productive and motivated when working from home
- The COVID-19 Pandemic: Managing the Impact
- Support for First Responders, Front Line Workers and Public Facing Employees
- Financial tips for your financial health
- Increases in Domestic Violence
- Those with family members in long-term care facilities
- COVID-19: Employee Fatigue, Isolation and Loneliness
Recall of Philips CPAP machines*
Last month, electronics company, Philips, issued a recall with Health Canada of some of its Continuous Positive Airway Pressure (CPAP), BiLevel Positive Airway Pressure (BiLevel PAP) devices and Mechanical Ventilators. The recall was issued due to a foam abatement within the machines that can become loose and cause potential health risks.
To qualify for repair or replacement of these devices, users must register their machine on the Philips website.
CPAP, BiLevel PAP devices and Mechanical Ventilators are eligible for coverage under an HCSA and under some Extended Health Care plans. Plan administrators may want to inform plan members of this recall if the devices are eligible for coverage under their plan.
-
April 2024 eNews
In this issue:
- Competitive – and easy – benefits plans for your small business clients
- Simplifying benefits enrolment for your clients*
- NEW time-off tracking tool from HRdownloads*
- Focus on benefits fraud: Protecting your clients’ plans from abuse*
Competitive – and easy – benefits plans for your small business clients
Supporting your small business clients can be a challenge. It’s tough to find a competitively-priced benefits plan with the features they want. Small business owners may also need more of your time – especially if this is their first benefits plan.
That’s why we created Equitable EZBenefits™, a benefits solution designed with the needs of small businesses in mind. With a range of plan design options and valuable embedded services for plan sponsors and plan members, EZBenefits is available for groups with 2 to 25 employees. And to make things simpler for you, we’ve created an Advisor Concierge Service exclusively for EZBenefits. Whether you have a question about submitting a quote request for a new client or an issue with an in-force client, our Concierge Service is your go-to resource for EZBenefits support.Don’t have any EZBenefits clients yet?
To learn more about EZBenefits, watch our video to learn more or view our brochure.Simplifying benefits enrolment for your clients*
Navigating the benefits enrolment period can be overwhelming – for you, your clients and their employees. It’s difficult to ensure all plan members complete the necessary paperwork before the enrolment deadline.
That’s why we offer our secure Online Plan Member Enrolment tool at no extra cost to plan sponsors. The tool simplifies the onboarding process for your clients and their plan members by eliminating the need for paper enrolment forms.
It also makes enrolment faster and easier for your clients by:- Reducing errors and rework that can occur due to spelling mistakes or missing information on paper forms; and
- Sending automatic enrolment reminders to plan members, resulting in fewer late applicants.
- Enrol in their benefits plan in just minutes from their computer or mobile device;
- Easily enter all their enrolment information, including dependent details, banking information for direct deposit of claim payments and details for coordination of benefits; and
- Designate their beneficiary electronically.
Ready to share our Online Plan Enrolment Tool with your clients? Get them started with these helpful resources:
- Online Plan Member Enrolment Flyer for Plan Administrators
- Online Plan Member Enrolment Quick Reference Guide for Plan Administrators
- Quick Reference Guide for Plan Members
To learn more about how Online Plan Member Enrolment can simplify benefits enrolment for your clients, contact your Group Account Executive or myFlex Account Executive.
NEW time-off tracking tool from HRdownloads*
Through our partnership with HRdownloads®, EZBenefits clients now have complimentary access to Timetastic —a time-off tracking tool that can make it easier to manage employee vacation time, sick days and more.
Timetastic integrates seamlessly with HRdownloads and includes a mobile app to help manage time-off requests from any mobile device.
To see Timetastic in action, check out this demo.
EZBenefits also includes other helpful resources and tools from HRdownloads that can make daily human resources tasks easier, including:- A robust, award-winning HR management platform (HRIS);
- HR documents, templates, compliance resources and articles; and
- A live HR advice helpline.
Learn more about accessing HRdownloads.Focus on benefits fraud: protecting your clients’ plans from abuse*
According to the Canadian Life and Health Insurance Association (CLHIA), benefits fraud costs insurers and plan sponsors millions of dollars each year, which can lead to increased premium costs.
Resources for your clients
Both plan administrators and plan members play a role in preventing benefits abuse. So, we’ve compiled some resources you can share with your clients to help them understand what benefits fraud is and how to prevent it:- CLHIA’s free 15-minute Protect Your Benefits online course for plan administrators and their members
- CLHIA’s Fraud is Fraud program, including their FAQs on benefits fraud
- Our online guide to benefits abuse
- Tips for plan administrators and plan members to protect their plan
How we’re fighting benefits fraud
Our Investigative Claims Unit (ICU) works to detect and eliminate benefits fraud. We use a variety of investigative techniques, including CLHIA-led industry tools to detect and eliminate benefits fraud:- Joint Provider Fraud Investigation Program: A robust program that allows insurers to collaborate on fraud investigations that affect multiple insurers;
- Data Pooling Program: An initiative that pools data between insurers and uses advanced artificial intelligence to further identify and reduce benefits fraud; and
- Provider Alert Registry: A registry that allows insurers to view the results of other insurers’ anti-fraud investigations into specific practitioners.
-
Equitable Life Group Benefits Bulletin – February 2022
In this issue:
- Update: Alberta biosimilar coverage changes*
- Preferred Biosimilar Program*
- Responding to Quebec’s biosimilar policy*
- Dental fee guide updates*
- Reminder: Review manual allocations for HCSAs and/or TSAs*
- Mental health resources for plan members*
Update: Alberta biosimilar coverage changes*
In 2022, Alberta’s provincial drug plan is adding four originator biologics to its Biosimilar Initiative. It has ended or will end provincial coverage of these drugs for some or all conditions, as follows:
Four originator biologics added to Alberta Biosimilar Initiative- Lovenox: Jan. 10, 2022
- Humalog: Feb. 1, 2022
- NovoRapid: April 1, 2022
- Humira: May 1, 2022
Patients 18 and over who are using these drugs for the affected conditions will be required to switch to biosimilar versions of the drugs to maintain coverage under the province’s government drug plan.
How we are responding to protect our clients
To help prevent this change from resulting in additional costs for our clients’ drug plans while still providing plan members with access to safe and effective medications, we will no longer cover these originator biologic drugs for plan members in Alberta.
Effective May 1, 2022, claimants currently taking these drugs will be required to switch to a biosimilar version of the drug to maintain coverage under their Equitable Life plan.
This is a continuation of the Alberta biosimilar switch program we launched last March, when the province first introduced its Biosimilar Initiative.
Do my clients need to take any action?
No action is required by plan sponsors. Plan members taking these targeted originator biologics will be contacted directly to allow them ample time to transition to a biosimilar. Any cost savings associated with the change will be factored in at renewal.
Groups that opted out of the biologic coverage changes we made last March will automatically be opted out of these coverage changes, as well as any future changes to our Alberta biosimilar switch program. This means that their drug plans will continue to provide coverage to existing claimants for any originator biologics we stop covering as part of our biosimilar program.
Advisors with clients who wish to opt out of our Alberta biosimilar program, or who previously opted out and want to opt back in, should speak to their Group Account Executive or myFlex Sales Manager.
Communication to plan members
We will be communicating these coverage changes with affected claimants in early March to allow them ample time to change their prescriptions and avoid any interruptions in their treatment or their coverage. Thus far, the transition to biosimilars, has been smooth and continues to be successful.
What is the difference between biologics and biosimilars?
Biologics are drugs that are engineered using living organisms like yeast and bacteria. The first version of a biologic developed is known as the “originator” biologic. Biosimilars are also biologics. Biosimilars are highly similar to the drugs they are based on and Health Canada considers them to be equally safe and effective for approved conditions.
Questions?
If you have any questions about this change, please contact your Group Account Executive or myFlex Sales Manager.Preferred Biosimilar Program*
As part of our ongoing efforts to help ensure the sustainability of your clients’ drug plans, we continue to engage in strategic partnerships with pharmaceutical manufacturers.
We are pleased to announce a partnership to make Hyrimoz our preferred biosimilar for Humira. This partnership will generate additional savings for plan sponsors.
Plan members will still have the choice to use Humira biosimilars other than Hyrimoz. However, in the absence of alternative sources of reimbursement, this may increase their out-of-pocket amount.
The Preferred Biosimilar Program will take effect March 1, 2022 for all new claimants across Canada who start using a Humira biosimilar. It will take effect May 1 for existing claimants in Alberta who switch to a Humira biosimilar, to align with changes to the provincial plan.
Questions?
If you have any questions about this change, please contact your Group Account Executive or myFlex Sales Manager.Responding to Quebec’s biosimilar policy
Last year, the Quebec government announced it is phasing out coverage of biologic drugs. Beginning April 13, 2022, patients in Quebec using originator biologics will be required to switch to the corresponding biosimilar covered on the province’s public plan in order to maintain coverage.
The following populations are excepted from this new policy:- Pregnant women, who should be transitioned to biosimilars in the 12 months after childbirth.
- Pediatric patients, who should be transitioned to biosimilars in the 12 months after their 18th birthdays.
- Patients who have experienced two or more therapeutic failures while being treated with a biologic drug for the same chronic disease.
We are actively investigating the impact of this new policy on private drug plans in Quebec. We plan to implement further enhancements to our biosimilar programs in Quebec later this year to help prevent this change from resulting in additional costs for our clients’ drug plans. We will provide more details in the coming months.Dental fee guide updates
Each year, Provincial and Territorial Dental Associations publish fee guides. Equitable Life uses these guides to help determine the reimbursement limits for dental procedures. For your reference, below is the list of the average dental fee increases for general practitioners that will be used by Equitable Life for 2022.*
Dental fee guide increases over 2021*
*Data for all provinces and territories was not available at the time of publication. This chart will be updated on EquitableHealth.ca as more information becomes available.Province/Territory Average Fee Increase Alberta 3.9% British Columbia 7.35% Manitoba 5.79% New Brunswick 5.9% Newfoundland and Labrador 5% Nova Scotia 7.05% Northwest Territories 3% Nunavut 3.1% Ontario 4.75% Prince Edward Island 4.75% Quebec 5% Saskatchewan 5.99%
Reminder: Review manual allocations for HCSAs and/or TSAs*
If your client’s Health Care Spending Account (HCSA) and/or Taxable Spending Account (TSA) has manual allocations, they need to allocate these amounts to plan members each year. Please review all your plan members’ profiles on EquitableHealth.ca to ensure they have received their allocation(s) for the current benefit year.
If your clients have Plan Administrator update access on EquitableHealth.ca, they can update these amounts online by doing the following:- Select “View certificate”
- Select “Health Care Spending Account” or “Taxable Spending Account”
- Select “Update Allocation” in Task Center
- Enter amount in “Revised Allocation Amount”
- Override Reason – “Plan Administrator Request”
- Select “Save”
- Select “Reports”
- Select “New”
- Select “Next”
- Select “HCSA” or “TSA Totals by Plan Member”
- Select “Next”
- Enter end date of “12/31/2020”
- Select “Next”
- Select “Finish”
- View “Report”
Mental health resources for plan members*
As the COVID-19 pandemic continues to evolve, many Canadians are experiencing increased levels of stress, anxiety, and depression. Through our partnership with Homewood Health®, all of our clients and their plan members have access to a number of health and wellness resources designed to provide guidance and support. These resources include a number of webinars which discuss various COVID-19 and mental health-related topics. The webinars are pre-recorded so plan members can stream them at their convenience.
Understanding the Impact of COVID-19 on Your Mental Health
English webinar
French webinar
COVID-19: Loneliness & Isolation Fatigue - Self-Care Strategies
English webinar
French webinar
COVID-19: Dealing with Seasonal Affective Disorder
English webinar
French webinar
Reducing Anxiety & Managing the Transition Back to the Classroom - for Teachers
English webinar
French webinar
COVID-19: Specialized Mental Health Support for Health Care Professionals
English webinar
French webinar
COVID-19: Supporting Children’s Mental Health
English webinar
French webinar
Additional resources, including articles, tools, videos and podcasts, are available at Homeweb.ca/Equitable. Please encourage your clients to share these resources with their plan members.
-
Policy endorsement: Long Term Disability pre-existing condition period
We are updating our contracts to clarify how we handle the Long Term Disability (LTD) pre-existing condition period for employees returning from maternity or paternity leave.
A new LTD pre-existing condition period will no longer apply when an employee re-enrols in the benefits plan after their maternity or paternity leave ends, provided that they return to work on the date agreed upon with their employer, or in the time period allowed by the Employment Insurance Act, whichever is earlier.
To facilitate this change, we are amending some of the wording in our contracts and booklets, effective March 1, 2020. Below are links to the Endorsement to the Master Policy and the Summary of Master Booklet Wording Changes for this amendment. Please download and save these policy endorsement documents for your files.
In addition, please remind your clients to provide all of their plan members with a copy of the Summary of Master Booklet Wording Changes.
The next time your clients amend their benefits plan, the updated wording will be included in their group benefits plan booklets.
Download Endorsement to the Master Policy
Download Summary of Master Booklet Wording Changes -
Extending Homeweb to plan members who are losing coverage
We know these are difficult times for Canadian employers and their employees.
As businesses temporarily suspend operations to help stop the spread of COVID-19, some employers have had to make the difficult decision to temporarily lay off employees or put their benefits coverage on hold.
So we are pleased to announce that Homewood Health® and Equitable Life® will extend access to Homeweb, a personalized online mental health and wellness portal, for up to 120 days for plan members who have temporarily lost their benefits coverage due to COVID-19.
Employees and their family members will continue to have access to the Homeweb website and mobile app, including:
- iVolve, Homewood’s online self-directed Cognitive Behavioural Therapy treatment tool to help manage mild to moderate anxiety and depression;
- Resources and information to support themselves and their family members through the COVID-19 pandemic;
- An interactive online Health Risk Assessment to help identify and address health risks; and
- An online library of interactive tools, assessments and 20 different e-courses that allow each user to learn at his/her own pace.
This will allow businesses undergoing financial hardship to provide some support to employees who are temporarily without benefits coverage.
-
Redefine online surfing with Equitable Life
Conquer the tailslide of RSP season with direct deposits to your client’s Equitable Life plan from a financial institution’s online banking.
Learn more -
Equitable Life Group Benefits Bulletin - November 2022
The importance of timely plan member eligibility updates*
Effective Dec. 1, 2022, we are implementing a revised process for managing plan member and dependent health and dental claims that have been incurred and paid after coverage has been terminated. This new process is consistent with industry practices.
If health or dental claims have been incurred and paid after a plan member’s termination date but before we received notice of the termination, we will align the plan member’s or dependent’s termination date with the service date of the last paid claim, retaining premiums up until that date.
If no claims have been incurred and paid after the termination date, Equitable Life will process the termination as requested and refund any excess premium, subject to a maximum premium refund credit of three months.
Currently, we process the termination as requested and attempt to recover any claim overpayments directly from the plan member. We then refund any excess premiums that have been paid, subject to the maximum refund credit amount.
To avoid claims being incurred and paid after a plan member’s termination date, it is important for your clients to update plan member and dependent eligibility dates on or before the effective date of the change.
If you have any questions about the process your clients should follow for updating plan member eligibility, please contact your Group Account Executive or myFlex Sales Manager.QuickAssess®: Absence and accommodation request review services*
It can be difficult to navigate chronic or complex cases of absenteeism or accommodation requests. That’s where QuickAssess® can help.
QuickAssess is an optional, fee-per-use service that can provide your clients with an unbiased, timely assessment of complex plan member absences and workplace accommodation requests. Our disability experts can provide recommendations to help your clients manage:- Workplace absences
- Chronic or patterned absenteeism
- Requests to modify workplaces or duties
- Return-to-work coordination
- Employee Insurance sick leaves
For more information on using QuickAssess, including eligibility requirements, please contact your Group Account Executive or myFlex Sales Manager.
**Within two business days of receiving a completed QuickAssess Absence and Accommodation Review Referral Form and all required information. For more complex referrals, more time will be required.Finding a health care provider with TELUS eClaims direct billing*
By visiting TELUS’s Find a Provider page, your clients’ plan members can now easily search for paramedical and vision providers who are registered on the TELUS Health eClaims network and who can submit claims directly to us on behalf of their patients. Searches can be filtered by postal code to help plan members find the most convenient provider options.
As our direct billing provider for pharmacy, vision and paramedical claims, TELUS Health has an extensive network of 70,000 health care providers that provide direct billing to streamline the claims process.
Please note, plan members should always check Equitable Life’s list of de-listed providers before selecting a health care provider. The list is available for your clients and their plan members on EquitableHealth.ca, and is updated regularly.
For more information about TELUS eClaims, please contact your Group Account Executive or myFlex Sales Manager.First phase of the Canada Dental Benefit proposed for Dec. 1, 2022*
The federal government’s new Canada Dental Benefit is proposed to take effect on Dec. 1, 2022, subject to Parliamentary approval. The program will cover eligible expenses retroactive to Oct. 1, 2022, and this first phase would apply to Canadians under 12 years of age.
If implemented, the Canada Dental Benefit will provide dental care to Canadian families with under $90,000 adjusted net income annually. By 2025, the federal government expects to extend the benefit to children under 18, senior citizens and Canadians with disabilities.
Parents or guardians will be required to apply for this coverage through the Canada Revenue Agency (CRA) and must not have private dental coverage for the child(ren).
This new program will have no impact on your clients’ dental coverage and no action is required on their part.
* Indicates content that will be shared with your clients.
-
New flexibility with Equitable’s Term Exchange option
Great news! Equitable® has just added our Term 30/65 plan as an option for term exchanges! This gives clients greater flexibility to choose a term plan that can adapt to their specific needs.
Clients can exchange their Equitable 10-year or 20-year term plans to a Term 30/65 plan as their financial needs change – without additional underwriting.
What you need to know:
• A term plan that is a result of an exchange option cannot be exchanged again
• Exchange is available between the 1st and 5th coverage anniversary.
o Only up to the insured’s 65th birthday for exchange to T20
o Only up to the insured’s 55th birthday for exchange to T30/65
• To request a term exchange, use the Term Exchange form.
For additional information, refer to the Term Advisor Admin Guide on EquiNet®, or contact your Equitable wholesaler.
® or TM denotes a trademark of The Equitable Life Insurance Company of Canada.
