Site Search
378 results for pre-authorized debit plan
- About
-
An update on Travel Assist coverage
The last several months have been very difficult for plan members. We recognize how important it is for them to get back to a sense of normalcy, including making summer travel plans.
As countries start to reopen their borders, plan members with Travel Assist emergency medical benefits may have questions about whether they will be covered while travelling.
For plan members who want to travel outside of Canada, here’s what they need to know.
Out-of-country travel
Plan members travelling to countries that are popular vacation destinations and have reopened their borders will be covered for eligible expenses, including those related to COVID-19.
Please note: While a country may be open for travel, plan members should contact Allianz before departing to confirm that they are covered for travel to their specific destination.
Plan members travelling to countries for which the Government of Canada has issued a Level 4 travel advisory (“Avoid all travel”) will not be covered.
Please note that every country has different travel restrictions. Travelers could be denied entry to another country, even though their travel may be considered essential. Or they may be forced to self-isolate when they arrive at their destination. Canadians travelling to another country should consult that country’s travel restrictions and guidelines before departure and re-entry into Canada.
Communicating with plan members
Below is a link to a plan member version of this communication. Please encourage your clients to share this with their plan members who have Travel Assist coverage on their benefits plan. It’s important for them to know their coverage details before they make their travel plans. We have also posted this update on the plan member website at EquitableHealth.ca.
An update on Travel Assist coverage PDF
If you have questions, please contact your Group Account Executive or myFlex Sales Manager.
- [pdf] Life Quick Reference Guide
- [pdf] Now it’s even easier to grow your savings online!
-
Insights from a pandemic: Drug trends during COVID-19
We were expecting drug costs to rise this year due to the increase in “specialty” drugs, the shift to more expensive treatments for common conditions, and the introduction of new, costly medications. The COVID-19 pandemic has caused drug costs to rise even more than expected. While this was partly due to increased claims for certain drug categories, the most significant factor was the increase in dispensing fees as the provinces imposed 30-day refill limits.
Costs and claimants surge, drop, then climb again
Initially, as COVID-19 started to spread, we saw an overall spike in the volume and paid amounts for drug claims in March as plan members rushed to stock up on their medications. On our block, the average amount paid per certificate increased 16% in March, compared with the previous year.
This spike was followed by a drop in April after most provinces put 30-day refill limits in place. This led to a decrease in both average paid amounts and quantity per claim as people were limited to smaller refills. But the dispensing fee portion of drug cost tripled for many plan members who had to refill their prescriptions every month instead of every 90 days.
The April plunge was short-lived. Drug claims started to climb again in May as some provinces removed their 30-day refill limits. We’ve seen a continued increase so far in June as all remaining provinces have lifted their 30-day limits.
Claims for “specialty” drugs increase
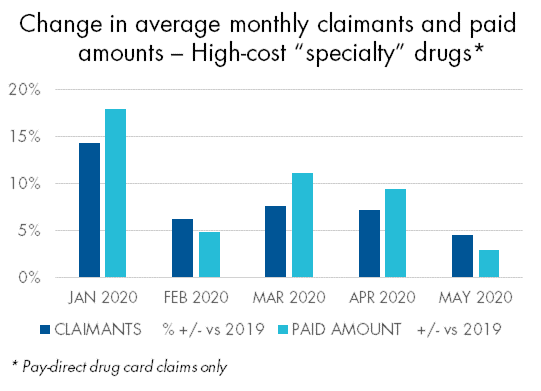 There were some notable exceptions to this trend. For example, both claimants and paid amounts for high-cost “specialty” drugs increased in March, April and May. Thirty-day refills are the norm for these drugs, so they weren’t impacted by the re-fill limits.
There were some notable exceptions to this trend. For example, both claimants and paid amounts for high-cost “specialty” drugs increased in March, April and May. Thirty-day refills are the norm for these drugs, so they weren’t impacted by the re-fill limits.Claims for asthma drugs had the largest surge of any common disease category in March but had no subsequent drop in April. Not surprisingly, claims for mental health drugs increased throughout the pandemic, including a 33% increase in the number of claimants in May.
Going forward, we should see the average quantity per prescription stabilize in future months and return to normal, provided pharmacies return most patients to refills of more than 30 days.
The full impact of COVID-19 remains to be determined. We will continue to provide timely updates on any developments that impact our clients and their plan members or their benefits coverage. In the meantime, please contact your Group Account Executive or myFlex Sales Manager if you have questions.
- Par Whole Life Summary
-
Equitable Life Group Benefits COVID-19 Update
The test of a great partner is one who stands tall when you and your clients need to rely on them most. As the COVID-19 pandemic continues, we thought you might find it helpful to have a summary of where we are during this crisis.
You can download this PDF version to refer to when meeting with your clients.
We are here with you and for you
We’ve taken several steps to support you, your clients and their plan members during this crisis, including:
- Providing premium refunds for insured, non-refund Health and Dental benefits;
- Waiving the waiting period for short-term disability claimants who tested positive for COVID-19;
- Extending out-of-country travel coverage for plan members who were unable to return to Canada;
- Providing increased flexibility for premium payments; and
- Keeping you and your clients informed with timely Q&As and announcements, webinars, and insights into the impact of COVID-19 on benefits plans.
As well, to commemorate our 100th Anniversary this year, we donated $4.5 million to purchase and install a new MRI for Grand River Hospital. And we donated $50,000 – $10,000 each – to five charities in British Columbia, Alberta, Manitoba, Ontario and Quebec. For more information about our celebrations, check out our website at www.equitable100.ca.
We have adjusted our business to become digital
Our business is near 100% digital, so the vast majority of our employees are now working remotely from home and are fully functional. Since the pandemic began, our IT and operations teams have digitally enhanced more than 20 different processes and services to make it easier for us to integrate with our distribution partners in this new reality.
We pride ourselves on our customer service
In 2019, our dedication to customer service was recognized with outstanding survey results.
- In a 2019 survey of customers from 15 life insurance companies,1 Equitable Life ranked #1 on the Net Promoter Score, a measure used across industries to gauge the loyalty of a firm's customer relationships; and
- A survey of Group consultants, brokers and third-party administrators 2 ranked Equitable Life in the top two insurers across all categories.
For 2020, we continue to deliver service at the same level with no disruptions during this crisis. Our Customer Care Centre remains open to support plan members and can be reached at 1.800.265.4556. And our Client Relationship Specialists are available for Plan Administrator questions and support.
We are financially strong and stable
We remain financially strong and continue to focus on meeting the needs of Canadians. At the end of the first quarter, our Life Insurance Capital Adequacy Test (LICAT) ratio is at 152.5%, well above our goal and the regulatory requirement.
As the global situation continues to evolve, rest assured that Equitable Life is unwavering in our commitments to you and the communities we serve. We are here with you and for you. Please contact your Group Account Executive or myFlex Sales Manager if you have questions or need assistance.
1 LIMRA CxP Customer Experience Benchmarking Program, Life Insurance In-Force Experience 2019
2 NMG Consulting’s Canadian Group Benefits Survey 2019
-
On June 26, 2021 make room for more EDO room
Effective June 26, 2021, a term rider added to an Equimax Estate Builder® or Equimax Wealth Accumulator® policy may allow for an increase to the maximum Excelerator Deposit Option (EDO) payment limit.
Your clients who have a temporary insurance need and add a term rider to their Equimax plan may be able to take advantage of the additional exempt room and higher EDO payment limits to build the policy values. Make Equimax® your first choice for your clients’ whole life insurance needs.
Want more information?
Learn more about the changes and transition rules.
Contact your Regional Sales Manager for more information on these changes and other sales ideas.
-
2022 brings a new year of retirement savings opportunities
As a new year begins, you will start to reach out to your clients about the upcoming Retirement Savings Plan deadline, March 1, 2022. This year, connect with your clients through social media, video chats, emails or even in-person. Try Equitable’s Case Studies, Prospecting Letters, Video and Equitable Blog on EquiNet® to make the most of your meetings. Designed for each specific target group, these sales strategies can help initiate a conversation about retirement savings goals.
To learn more about Retirement Savings Plans, click here. -
January 2023 eNews
Responding to Saskatchewan’s biosimilar switch initiative*
We are changing coverage for some biologic drugs in Saskatchewan in response to the province’s biosimilar initiative. These changes will help protect your clients’ plans from additional drug costs that may result from this new government policy while providing access to equally safe and effective lower-cost biosimilars.
Saskatchewan’s provincial biosimilar initiative
Announced in October 2022, the Saskatchewan Biosimilars Initiative ends coverage of ten biologic drugs beginning on April 30, 2023.
Patients in the province who are using these drugs will be required to switch to biosimilar versions of these drugs by April 30, 2023, in order to maintain their Saskatchewan Drug Plan coverage.
Equitable Life’s response
To ensure this provincial change doesn’t result in your clients’ plans paying additional and avoidable drug costs, we are changing coverage in Saskatchewan for most biologic drugs included in the provincial initiative.
Beginning April 30, 2023, plan members in the province will no longer be eligible for most originator biologic drugs if they have a condition for which Health Canada has approved a lower cost biosimilar version of the drug.** These plan members will be required to switch to a biosimilar version of the drug to maintain coverage under their Equitable Life plan.
Communicating this change to plan members
We will inform any affected plan members in early February of the need to switch their medications so that they have ample time to change their prescriptions and avoid any interruptions in treatment or coverage.
What is the difference between biologics and biosimilars?
Biologics are drugs that are engineered using living organisms like yeast and bacteria. The first version of a biologic developed is known as the “originator” biologic. Biosimilars are highly similar to the drugs they are based on and Health Canada considers them to be equally safe and effective for approved conditions.
Questions?
If you have any questions about this change, please contact your Group Account Executive or myFlex Sales Manager.
**The list of affected drugs is dynamic and will change as Saskatchewan includes more biologic drugs in its biosimilar initiative, as new biosimilars come onto the market, and as we make changes in drug eligibility.
Ontario announces 2023 biosimilar switch program*
The government of Ontario recently announced the launch of a biosimilar initiative to switch patients from eight originator biologic drugs to biosimilar versions of the drugs.
Patients in Ontario using affected originator biologic drugs will have until December 29, 2023 to switch to a biosimilar version of their medications in order to maintain coverage under the province’s public drug plans.
We are actively monitoring and investigating the impact of this new policy on private drug plans in Ontario. We plan to implement changes to coverage of biologic drugs in the province in 2023 to help prevent this change from resulting in additional costs for our clients’ drug plans. We will provide more details in the coming months.
If you have any questions, please contact your Group Account Executive or myFlex Sales Manager.
Dental fee guide updates*
Each year, Provincial and Territorial Dental Associations publish fee guides. Equitable Life® uses these guides to help determine the reimbursement limits for dental procedures. For your reference, below is the list of the average dental fee increases for general practitioners that will be used by Equitable Life for 2023.***Dental fee guide increases over 2022***

***Data for all provinces and territories was not available at the time of publication. This chart will be updated on EquitableHealth.ca as more information becomes available.
Equitable Life ranks high with Canadian group advisors*
Equitable Life ranked second nationally and first in Ontario among major insurers in a recent survey of Canadian group benefits advisors.
NMG Consulting, a leading global consulting firm, conducted in-depth interviews with 130 leading group consultants, brokers and third-party administrators across the country between May and August 2022 for its annual Canadian Group Benefits Study. Based on these interviews, NMG ranked group insurers in six categories, ranging from operational management to technology.
Nationally, Equitable Life ranked either first or second in four of the six main categories:

Advisors in Ontario, in particular, scored Equitable Life very favourably. We ranked #1 overall in the province, finishing first in four of the six overall categories, including: Relationship Management, Operational Management, Underwriting and Claims Management and Technology.
“The fact that advisors regard us so highly in so many categories is a testament to our mutual status and our ability to focus exclusively on our clients and advisors,” said Marc Avaria, Senior Vice President of Group. “We are truly working together to build strong, enduring and aligned partnerships.”
“While we are happy with these results, we won’t rest on our laurels,” added Avaria. “We will continue to dedicate ourselves to providing our clients and advisors with a better benefits experience.”
Here are more of the highlights from this year’s results:
Nationally, we ranked first in all 10 subcategories in Operational Management, including:- Overall service to intermediaries,
- Overall service to plan sponsors,
- New quote process,
- Plan implementation,
- Renewal process,
- Information shared at renewal,
- Accuracy and timeliness of reporting and billing,
- Administration quality and responsiveness,
- Taking ownership and
- Management information quality and availability.
- Company relationship management,
- Ease of doing business,
- Account executive capability,
- Market knowledge,
- Visit/call quality,
- Effective coordination and
- Advice.
- Fairness and timeliness of disability claims (1st)
- Fairness and timeliness of health claims (2nd)
- Fraud management (2nd)
- Competitiveness of pooling charges (2nd)
- Group underwriting flexibility (3rd)
- Health and dental TLR competitiveness (3rd)
- Overall technology – Intermediary (2nd)
- Member experience (2nd)
